The first article to be considered in the present research paper is the work of Carol L. White, Nancy Mayo, James Hanley and Sharon Wood-Dauphinee (2003) titled “Evolution of the Caregiving Experience in the Initial 2 Years Following Stroke”. The purpose of the study of the present article is to identify the quality of life (QoL) and the health-related quality of life (HRQoL) of the caregivers who take care of people who had a stroke. The study includes research in the spheres of dependence of the results on gender and age peculiarities of participants of the research (White et al., 2003).
The influence was observed for 2 years (on a subset of data). Caregivers were initially interviewed about stroke survivors if those could not provide the information for the researchers conducting the Montreal Cohort Study on their own. As a result of such a scheme of study the additional information was received from caregivers only in such cases (White et al., 2003).
Caregivers constituting the main goal of the present study were continuously interviewed for the 2 years during which the research was conducted. Members were admitted only if the stroke survivor did not undergo treatment in any other rehabilitation center but under the supervision of the chosen stroke survivor. Besides, the caregiver should have begun taking care of the stroke survivor from the very beginning, i.e. right after the stroke. In another way, they were considered not eligible for the study (White et al., 2003).
The study was based on the exclusion criteria and the sample design constitutes a series of voluntary surveys. The probability technique is used in the described study. The consent rate was 48%, the mortality rate was 10%. 52% refused the participation in the survey for two identified reasons:
a) near-normal to the normal recovery of a stroke survivor, and caregiver stated that she/he was no longer in a caregiving role… b) caregiver reported being too busy in the role to respond to the interview (White et al., 2003).
15 participants did not stipulate their reasons for refusal.
The size of the sample was constituted 97 caregiver/stroke survivor dyads. Initially, these were 181 caregivers considered appropriate for the present study. However, 84 candidates either refused to continue the study or quit for other reasons being ineligible for the research. The sample size was adequate for the study as it was qualitative; all measures were thoroughly collected and analyzed.
After receiving the informed consent from both the caregiver and the stroke survivor the researchers confirmed cooperation with them shortly after leaving the hospital. The first interview was to be taken 6-7 months after the stroke. The next interview was taken 23 months after the stroke. These interviews took about 30-45 minutes and proved to be efficient because they were undertaken by specially trained professionals specializing in conducting telephone interviews.
It was an experimental study; nobody was manipulated because all participants were chosen according to similar criteria, the main criterion was a stroke and a caregiver who stayed with the stroke survivor. It was a purely theoretical study involving no control or experimental treatment. The only measures that were newly introduced in the study, marking it as innovative were the terms of QoL (quality of life) and HRQoL (health-related quality of life). These measures are considered central in the present study because the authors who initiated the study consider that more attention is paid to the issues of moral and emotional disorders caregivers face because of constant hardships and restraint accompanying providing care for the stroke survivor. However, using such variables as QoL and HRQoL one can come to a conclusion that not only the emotional but the physical status of the caregivers are deeply affected by the care they have to give to the stroke survivor. Thus, the authors insist on the necessity to study the overall health condition of the caregiver in a complex way.
In general, there were five data collection instruments used in the present study. It involved the application of the Barthel Index for measuring physical function. The second data collection instrument was a checklist of 24 symptoms caregivers could have experienced. The Burden Index was a tool applied to assess the stress associated with caregiving. HRQoL was assessed with the help of the Medical Outcome Study 36-Item Short Form Health Survey, a 0-10 numerical rating scale was the instrument used to measure the whole QoL variable.
The Barthol Index is a measure used to assess the functional condition of the caregiver with the help of a range of basic everyday activities such as “self-care, continence of bowel and bladder, and mobility” (White et al., 2003).
The measurement instrument generally included 10 items that can be ranged from 0 to 100. Survival, physical recovery, and restoration of functional activity, as well as discharge disposition, have been chosen as the validity of prediction of the present study. As for the interpretation of scores, the following scale was proposed as a standard: 60 or fewer points mean heavy dependence, 61-90 points mean the average level, above 90 points stand for slight dependence (White et al., 2003).
HRQoL was measured with the help of Medical Outcome Study 36-Item Short Form Health Survey shortly called SF-36. It is
A generic scale of perceived health status that includes eight multi-item scales measuring physical functioning, role limitations because of physical health problems, bodily pain, general health perceptions, vitality, social functioning, role limitations resulting from emotional problems, and mental health (White et al., 2003).
The data received on the basis of SF-36 may be subdivided into the physical and mental characteristics subscales, MCS and PCS. They are standardized, have a mean of 50 and a standard deviation of 10. Important aspects of the discussed instrument are the internal consistency of the study subscales and construct validity. Tables 1 and 2 illustrate the HRQoL scales SF-36.
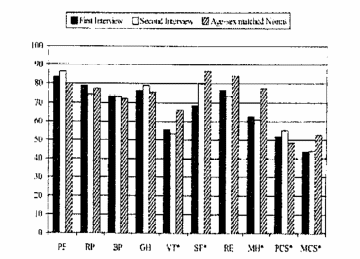
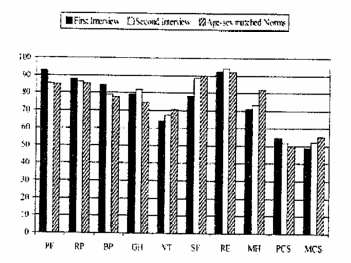
The overall, complex assessment of the results on an HRQoL model may be illustrated in Table 3.
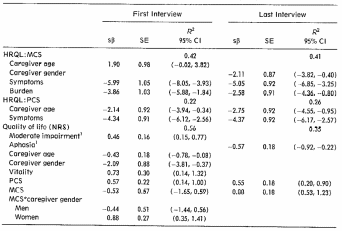
The study was conducted by means of telephone interviews twice in the whole period of the study. Consideration of the ethical side of the study was thoroughly taken care of by the researchers:
The study was approved by the research ethics committees of the participating hospitals. Informed consent was provided by all caregivers (White et al., 2003).
The second article to be considered in the present work by A. Elaine Bond, Christy Rae Lee Draeger, Barbara Mandleco and Michael Donnelly (2003) titled “Needs of Family Members of Patients With Severe Traumatic Brain Injury”. The purpose of the study was to understand and satisfy the basic needs of both the patients with severe brain injury – much research has been done in this sphere to define the needs they face while coming across a serious problem – the described category of patients are in an extremely unstable and unpredictable status, the death rate is very high, so the families of the patients face the unknown situation they at times cannot handle. The task of nurses is hence seen in providing adequate help not only to patients but also their families, including providing them with reassurance, comforting, timely and adequate information.
The sample was obtained among the families of patients of an 11-bed neurological ICU in a level one trauma center. The members of seven patients’ families were continuously interviewed during the stay of their relative in the trauma center with the purpose of defining their needs that remained unmet.
On each of the remaining days of a patient’s ICU stay, the patient’s family member was asked to describe the family’s needs and concerns and also was asked if any new needs had arisen. Subsequent interviews were conducted either at the hospital or by telephone, at the participants’ convenience, building upon the trust developed during the first in-person interviews (Bond et al., 2003).
The research was based on three inclusion criteria – the age of participants should have been more than 18 years old, the patient had a GCS score of 8 and more, and the patient’s time of hospitalization should have been a minimum of 24 hours. The design of the study was exploratory qualitative descriptive using the probability technique (Bond et al, 2003).
The consent rate was 100% among the seven chosen families. The mortality rate was five of seven patients. As it has already been mentioned, the sample size for this qualitative research was seven families of patients with severe brain injury – the sample seems to be inadequate for the study that should involve much more participants with varied backgrounds and individual characteristics to obtain more adequate information.
The study was conducted until the moment of obtaining all necessary information from the relatives, or with the death or discharging of the patient. Interviews were recorded on the videotape being transcribed verbatim afterward. The group of seven families was interviewed for 4 months from January to April 2001. The age ranged from 41 to 61 years (Bond et al., 2003). It was an experimental study.
The data collection instrument used for the present study was only one – conducting the interviews with the patients with the aim of indicating their changing needs. The interviews were based on the Molter study of the need’s families of patients with severe brain damage have. Table 4 is an illustration of varied approaches to the assessment of the patients’ needs.
Data collection was undertaken in the hospital or by phone, as it has already been noted. Besides, there have been taken multiple measures to provide the participants’ confidentiality. First of all, they all signed the consent forms that provided detailed information on what measures were taken to ensure anonymity and confidentiality (White et al., 2003). Besides, it is notable that all videotapes with interviews were processed to remove any chance for identification of the interviewees.

There has been much research on the issues of terminally ill people and the appropriate caregiving they should receive. However, the focus on the caregivers and their life has also been paid much attention to recently – for example, Sandra M. Walsh, Griselle B. Estrada and Nancy Hogan (2004) indicate in their article that caregivers become the central characters in the discussed process, neglecting their own health and sacrificing their lives for the sake of the patients. In addition to the discussion of the second article, it is appropriate to mention the work of E. Latimer (1991) in which adequate communication of information about the patient’s state of health is discussed as an important issue of the philosophy and ethics of dealing with seriously ill and dying patients. The article of Kevin Brazil, Tom Abernathy, Patrick Critchley, Paul Crueger, Lynne Lohfeld, Kathleen Willison, Michelle Caron O’Brien, Mary Hode and H. Gayle Edward is also focused on the extended research of handling terminally ill and dying people that should include both the patients and the caregivers.
References
Bond, E.A. et al. (2003). “Needs of Family Members of Patients with Severe Traumatic Brain Injury”. Critical Care Nurse, Vol. 23, No.4, pp. 63-74.
Brazil, K. et al. (2002). Care of the Seriously Ill in the Community.
Latimer, E. (1991). Caring for seriously ill and dying patients: the philosophy and ethics.
Walsh, S.M. et al. (2004). Individual telephone support for family caregivers of seriously ill cancer patients.
White, C.L. et al. (2003). “Evolution of the Caregiving Experience in the Initial 2 Years Following Stroke”. Research in Nursing & Health, 26, pp. 177-189.