Introduction / outline of the research
One of the most peculiar aspects of a post-industrial living is the fact that, as time goes on, more and more people grow increasingly comfortable with the process of Western health care paradigm incorporating a number of unconventional approaches towards addressing patients’ health problems, closely associated with the concept of complementary and alternative medicine – CAM (Bishop, Yardley and Lewith, 2006). Such state of affairs appears to be of a clearly phenomenological essence. After all, even up to this date, there are no universally accepted definitions of a complimentary/alternative therapy in existence.
Therefore, in order to ensure this study’s ideological unbiasedness, during the course of conducting its consequential phases, we will make a point in utilizing Leckridge’s (2004) definition of CAM, as such that is being discursively neutral, “CAM is a group of non-orthodox and traditional therapies that may be used alone, or to complement orthodox or other non orthodox therapies, in the treatment and prevention of disease in human patients (p. 413). Another reason, why we have chosen in favor of resorting to the earlier mentioned definition of CAM, is that it is being implicitly suggestive of what can be considered the varying extent of complimentary therapies’ procedural appropriateness/inappropriateness.
As of today, it became a commonplace practice among health care professionals to adopt an ambivalent approach towards conceptualizing CAM’s detrimental and beneficial effects (Baarts and Pedersen, 2009). The reason for this is apparent – as of today, not even a single scientifically substantiated proof of complementary/alternative therapies’ practical effectiveness has been obtained. This is because CAM’s clinical trials usually produce inconclusive and often diametrically opposite results (Shang et al. 2005).
However, it would be quite inappropriate to consider the very concept of CAM therapy as being innately conflicting with the methodological premise, upon which the proper functioning of today’s health care system is being based. This is because modern principles of a Western medicinal education also appear fully correlative with the practice of subjecting patients to the alternative/complimentary treatments. Moreover, the growing popularity of alternative/complimentary therapies also appears being thoroughly consistent with the implications of recent bio-medicinal discoveries, which had taken place during the course of last few decades, and which confirm the existence of dialectical links between the workings of a particular patient’s psyche and the subtleties of his or her health-condition (Park, 2002; Levack, 2009).
The methodological approach, towards substantiating the validity of an earlier outlined thesis, will consist of the following major components: a) the review of the relevant academic literature, b) the collection of a questionnaire-based empirical data, in regards to the qualitative essence of sampled students’ attitudes towards the discussed subject matter, c) the discussion of an obtained data’s theoretical and practical implications. We expect to find a strong enough theoretical and empirical evidence as to the fact that pharmacy students’ academic curriculum should indeed include a course on the significance of CAM therapies.
Review of previous research
Even though it became a commonplace practice among certified physicians to refer to patients’ predisposition towards the use of CAM as being of an essentially irrational nature, such point of view cannot be considered as representing an undeniable truth-value. The reason for this is simple – there is a plenty of evidence as to the fact that many patients’ tendency to resort to the use of CAM comes as a result of their dissatisfaction with having been previously subjected to the orthodox medicinal therapies (Kayne, 2009). In its turn, this can be explained by the fact that orthodox medicinal practitioners are known to rely upon a ‘conveyer-belt’ approach towards addressing their professional duties. (Reast, Palihawadana & Dayananda, 2008).
Apparently, as time goes on, the innate inadequacies of orthodox therapies are being increasingly perceived as such that are being metaphysically inconsistent with the very paradigm of an effective health care (Bakx, 1991). Thus, it will only be logical to assume that the growing popularity of complimentary therapies has in part to do with the fact that, unlike what it is being the case with conventional therapies; they are based upon an individual-centered methodology towards addressing patients’ health problems (Kayne, 2009). This, of course, is being suggestive that, contrary to what is being implied by CAM’s critics, there are no good reasons to think of patients that seek CAM therapies as being irrationally minded.
According to the findings of Astin’s (1998) study, conducted over the sample of 1035 randomly selected CAM users, one of the foremost predictors of people’s positive attitude towards complimentary/alternative therapies was determined their possession of a university diploma. Apparently, thoroughly educated people are being naturally predisposed towards favoring individual-centered therapies, which are being strongly associated with CAM.
This brings us to discuss the validity of another major criticism of CAM therapies, concerned with suggestions that the effectiveness of these therapies is being rarely evaluated by the mean of subjecting them to clinical trials. For example, according to Colquhoun (2007), the reason why The National Institute for Health and Clinical Excellence (NICE) is not being required to evaluate the effectiveness of CAM, in order for this type of medicinal products to be licensed, is that the beneficiary effects, induced by CAM, are assumed to be reflective of an affiliated placebo effect. In other words – CAM’s healing powers are being of essentially fictitious essence.
Nevertheless, a closer analysis of what accounts for the process of conventional medications’ licensing also implies that there are no good reasons to consider the successful completion of a clinical trial, concerned with evaluating the actual effects of a particular drug, as a guarantee that this drug will necessarily benefit its users. This is because pharmaceutical companies are being naturally interested in doing just about all just it takes, in order for this drug to be allowed for sale in pharmacies – even at the expense of withholding information about the full scope of a newly developed drug’s side effects (Colom & Vieta, 2011; Lary et al., 1999). This, of course, once again points out to the process of Western patients becoming increasingly comfortable with the very concept of CAM, as such that has been dialectically predetermined.
This paper’s thesis can be further supported even in regards to the ideas, contained in Jobst, Shostak and Whitehouse’s (1999) article. According to these authors, it is not only that a particular disease should not be thought of as something that needs to be eliminated at any cost, but also as such that often extrapolates the affected individual’s ability to remain healthy – whatever improbable it may sound. Therefore, conventional physicians’ tendency to prescribe patients with heavy doses of drugs, even when the treatment of flu is being concerned, cannot have a positive effect on these patients’ health condition, by definition. CAM therapies, on the other hand, are based upon a ‘holistic’ disease-treatment methodology. That is, they refer to the premise that, in order for a particular illness to be successfully addressed, physicians may never cease being observant of how this illness reflects a concerned patient’s overall state of physical well-being, which in turn is often being reflected by the particulars of his or her lifestyle (Pietroni,1987)
The appropriateness of an idea that students should be provided with an opportunity to learn about CAM therapies can also be explored in regards to another qualitative shift within the paradigm of a Western health care, which is taking place as we speak. This shift is being concerned with Western policy-makers’ increased tendency to discuss people’s ability to enjoy high quality health care services in terms of a privilege, rather than in terms of a constitutionally guaranteed right (Kelner et al., 2006). Therefore, it will only be logical to assume that, as time goes on, CAM therapies will continue to become ever more appealing to those who understand that the concept of ‘healing’ is being discursively superior to the concept of ‘curing’ (Finkler, 1994).
We believe that the insights, gained through the course of conducting the provided analytical review of relevant literature, do support the legitimacy of this study’s initial hypothesis as to the fact that pharmacy students should indeed be taught about complimentary therapies.
Aims, objectives, hypothesis
The foremost aims of this study can outlined as following:
- To substantiate the soundness of an idea that pharmacy students should be provided with an opportunity to learn about complimentary therapies, as an integral part of their academic curriculum.
- To confirm the appropriateness of a theoretical premise, upon which CAM therapies are being based.
- To expose the fallaciousness of an assumption that the improvement of patients’ physical condition, which often comes as a direct result of CAM therapies’ deployment, is being solely concerned with a placebo effect.
These aims predetermine the qualitative essence of study’s objectives, which in turn can be defined as follows:
- To expose what may account for societal, educational and pharmacological benefits of pharmacy students being prompted to learn about complimentary therapies.
- To obtain the empirical (survey-based) evidence as to the fact that pharmacy students would be comfortable with the idea of being required to attend a course on CAM therapies.
- To outline the possible vector of future researches, in regards to the measurable effects of pharmacy students being required to gain theoretical and practical knowledge of CAM therapies.
The hypothesis of this study’s empirical phase is that, the survey of sampled pharmacy students’ attitudes towards the concept of complimentary therapy, must be suggestive of their emotional comfortableness with the idea that a course on CAM should be incorporated in their academic program.
Methodology, description of procedures
Given the clearly defined longitudinal subtleties of this study’s subject matter, it will only be logical, on our part, to choose in favor of the utilization of a method of qualitative inquiry throughout this study’s empirical phase. After all, the deployment of a qualitative research methodology has been proven especially suitable within the context of conducting studies where the exploration of a significance of subject-related psychological aspects constitutes an important element of a research-process (Rubin & Rubin, 1995). Hence, qualitative research’s key features:
- This type of research always stresses out the importance of assessing the studied phenomena through the eyes of those affected by this phenomena the most. In its turn, this provides researchers with an additional insight into phenomena’s qualitative characteristics.
- The methodology of a qualitative research allows researchers to identify social circumstances, which affect the spatial emanations of a studied subject matter.
- The utilization of a qualitative research’s methodology, within the context of researchers striving to gain a three-dimensional insight into the actual essence of an investigated phenomena, allows them to determine the extent of phenomena’s objectiveness/subjectiveness.
- The methodology of a qualitative research allows researchers to adopt an intellectually flexible approach towards conducting a social inquiry, which in turn allows them to modify research-procedures, as they see fit.
This study’s utilization of a qualitative research-methodology will also feature the elements of a quantitative research. That is, after having collected the empirical questionnaire-based data, we will subject it to a percentile wise quantification (Franses & Paap, 2001).
The instrument of collecting data, relevant to this study’s subject matter, is the questionnaire containing nine questions that are being expected to elicit discursively valid responses from study’s participants. Out of these nine questions, five (questions: 1, 3, 5, 6, 7) were designed to provide us with a longitudinal insight into selected students’ attitudes towards the idea of studying CAM therapies. The other four sub-questions (2, 4, 8, 9) were designed to supplement this insight with the relevant demographic information.
This questionnaire will handed to hundred fifty 1st, 2nd, 3rd , 4th, and 5th year pharmacy students that currently study at Bradford University. These students will be asked to fill out the provided questionnaire and to return it within a matter of one week. The proposed hypothesis will be deemed legitimate if the analysis of the obtained responses reveals a positive attitude towards the idea that pharmacy students should study CAM therapies, on the part of more than 50% of participants.
Results or Key Findings
Out of 150 students that were asked to fill out the survey-questionnaire, all 150 of them provided a feedback to the contained nine questions.
Question 1
Out of all respondents, 22% of first year students, 69% of second year students, 65% of third year students, 86% of fourth year students, and 92% of fifth year answered this question positively.
Table 1
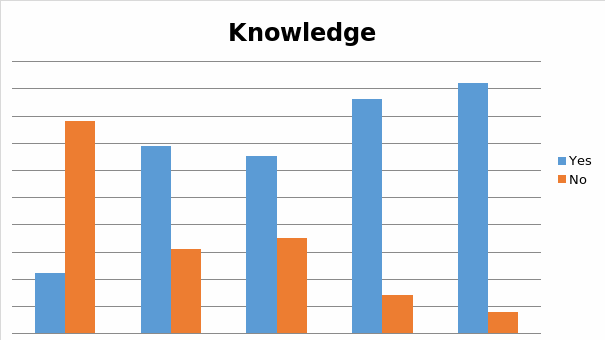
Question 2
As it can be seen on Table 2, it were specifically Hebral medicine, Chinese medicine, Accupuncture, Homeopathy and Aromatherapy, which scored the highest on the scale of parfticuipants’ awareness about CAM.
Table 2
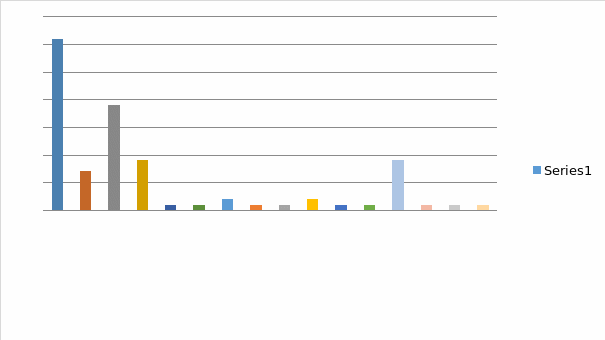
Question 3
This question was answered positively by 13% of first year students, 35% of second year students, 42% of third year students, 34% of fourth year students, and 43% of fifth year students.
Table 3
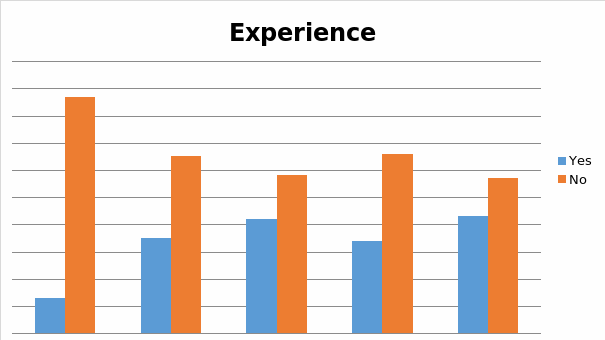
Question 4
The responces, provided to this particular question, suggest that it is specifically Herbal medicine, Accupuncture and CBT, with which most students expressed themselves being experientialy familiar.
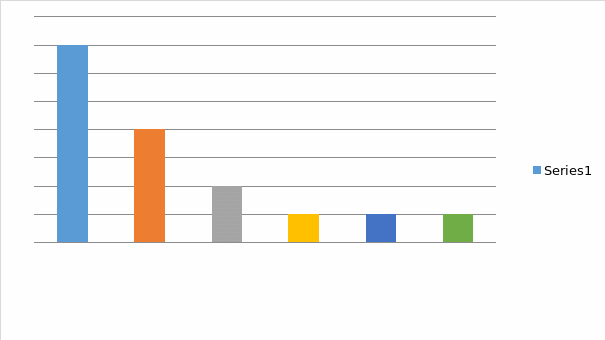
Question 5
Participants’ responses to this question (concerned with students’ being asked to rank CAM’s therapeutic value on the scale from one to five), reveal that it were namely first year, third year and fifth year students, who have overwhelmingly chosen in favor of ranking CAM’s value as such that is being neither too low nor too high. On the provided scale, CAM’s value scored the highest with second year students.
Table 5
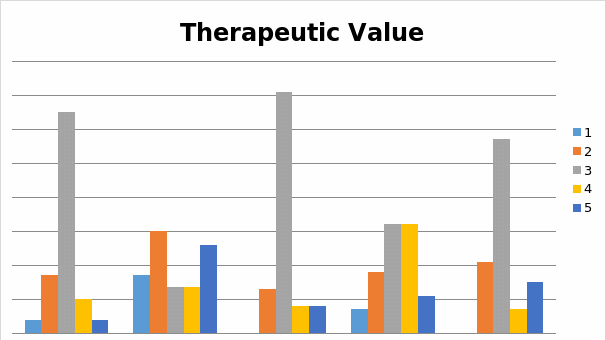
Question 6
Participants’ responses to this question suggest that it is specifically third year students who appear to be the most comfortable with the idea that the course on CAM medicine should be made an integral part of their learning.
Table 6
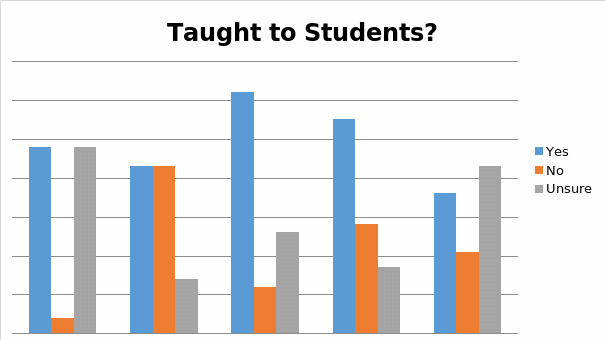
Question 7
Participants’ responses to this question indicate that it is primarily third and fourth year students who favored the suggestion that patients will indeed be able to benefit from being exposed to CAM therapies.
Table 7
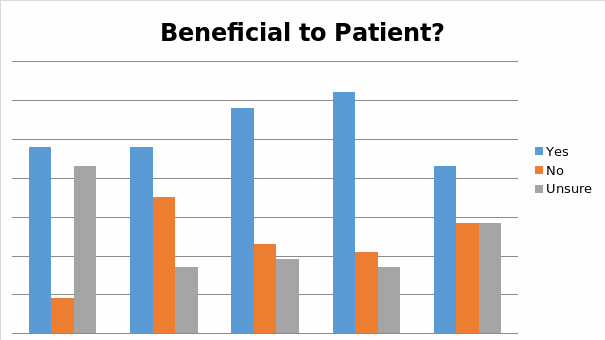
Question 8
Participants’ responses to this question reveal weakly defined margins between the numbers of first year, second year, third year, and fourth year students, who agreed to take part in the survey. The margin, concerned with the number of fifth year students, appears rather being rather significant.
Table 8
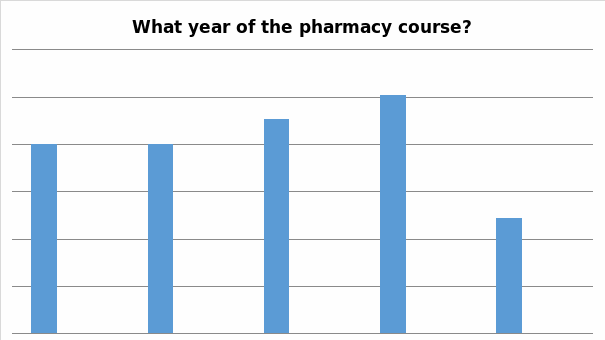
Question 9
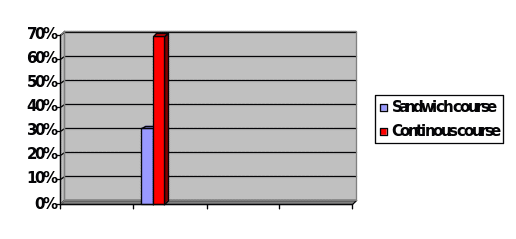
Participants’ responses to this question suggest that; whereas, 31% of surveyed students take pharmacy as a sandwich course, 69% of students study pharmacy on a continuous basis.
Table 9
Are you part of the sandwich course or the continuous?
Discussion
The analysis of the received responses’ implicational significance, allows us to come up with a number of discursive insights, in regards to this study’s empirically obtained data:
- Given the qualitative essence of participants’ responses to Question 1, it appears that the extent of students’ awareness of CAM relates to the number of years, they have spent studying pharmacy, in a positive progression. The validity of this statement appears being slightly inconsistent with the fact that, as it can be seen in Table 1, the participated third year students scored slightly lower on the CAM-related knowledge scale than the participated second year students. This inconsistency, however, may well be of a purely technical nature. After all, the provided responses do suggest a steady rise of students’ awareness of CAM, reflected by the measure of their seniority.
- Students’ responses to Question 2 suggest an undeniable fact that most of them do think of the application of CAM therapies as such that is being well capable of providing patients with an immediate pain-relief. At the same time, these responses indicate students’ lessened awareness of CAM therapies’ ability to provide patients with the long-term ‘healing’ benefits. This, of course, can be explained by the fact that, while studying in Britain, these students never cease being encouraged to apply an essentially euro-centric approach towards evaluating a particular therapy’s benefits. In its turn, this is being suggestive of the fact that, while recognizing CAM therapies’ potential ability to benefit patients in a variety of different ways, these students’ very affiliation with the orthodox pharmacological methodology, naturally causes them to think of CAM as such that represents a supplementary medicinal value.
- Given the qualitative essence of students’ responses to Question 3, we can be quite sure as to the fact that, in full accordance with this study’s initial thesis, the extent of students’ experiential familiarity with CAM therapies positively relates to the number of years they have spent studying pharmacy. At the same time, however, these students’ pursuance of their educational agenda alone cannot be thought of as a sole contributing factor towards their ever-increased awareness of CAM. Apparently, as time goes on, students are being naturally exposed to the situations when they, or the members of their families, end up choosing in favor of a particular CAM therapy.
- The qualitative essence of students’ responses to Question 4 is being discursively consistent with the qualitative essence of their responses to Question 2. That is, students’ responses to both of these questions suggest that it is specifically CAM therapies’ ability to provide patients with the immediately-felt beneficiary effects, which students consider as such that is being reflective of these therapies’ foremost value. This, of course, is being reflective of participants’ tendency to view CAM from rather a ‘functional’ then a ‘holistic’ perspective.
- Given the qualitative/spatial subtleties of students’ responses to Question 5, we can hypothesize that, while studying pharmacy, students are being simultaneously exposed to the instances of application of CAM therapies proving utterly effective, on the one hand, and rather ineffective, on the other. This is the reason why it is specifically first, second and third year students, who have overwhelmingly chosen in favor of ranking CAM’s therapeutic value as such that is being neither too low nor too high. Whereas; the ranking of CAM’s value, on the part of first year students, appears being reflective their awareness of currently predominant CAM-related discourse, the third and fifth year students’ tendency to assign the numerical value 3 to what their perceive as the extent of CAM therapies’ effectiveness, appears being more reflective of their experiential knowledge, in this respect. Moreover, it is also being reflective of their tendency to evaluate CAM therapies’ effectiveness in regards to how these therapies’ practical application may provide patients with the immediately felt benefits.
- The analysis of students’ responses to Question 6 points out to the fact that, as time passes, students tend to adopt qualitatively different attitudes towards the idea that the course on CAM should be included, as a part of their studies. For example; whereas, only 4% of first year students provided a negative feedback to this particular question, the percentage of second year students, who did not agree with the idea, accounted for 43%. As compared to what it is being the case with third and fourth year students, fifth year students also appear being somewhat less enthusiastic about the proposition, contained in the question. Nevertheless, the strongly defined disparities about students’ attitudes towards the idea that the course on CAM should be made a part of their pharmacological studies, do not seem being reflective of respondents’ actual stance on the issue, as much as they are being reflective of the fact that, as practice indicates, it is specifically second and fifth year students who experience a particularly hard time, while coping with academic assignments.
- Students’ responses to Question 7 suggest that, while studying pharmacology, they grow increasingly comfortable with the idea that the practice subjecting patients to CAM therapies is being thoroughly appropriate, because patients do benefit from it. The fact that only 43% of fifth year students answered this question positively is being somewhat inconsistent with the overall trend (seen in Table 7) that, as time passes, students appear becoming ever more acknowledgeable of CAM therapies’ beneficiary effects on patients. This inconsistency, however, may well have to do with the fact that, while nearing the time of their graduation, fifth year students grow somewhat cautious about supporting the ideas that are being incompatible with the orthodox healthcare paradigm, as they think that it might impair their chances of becoming graduated.
- Students’ responses to Question 8 point out to the fact that the relevant insights, gained through the process of conducting this study, can be indeed defined as spatially representative. This is because, as it can be seen in Table 8, the percentile margins between the groups of first, second, third, and fourth year students are not being prominently delineated. Even though that, as it can be seen in Table 8, the percentage of fifth year students accounted for only 12%, this did not substantially affect the cross-sectional value of students’ responses.
- The fact that, as it can be seen in Table 9, 31% of students described themselves as such that study pharmacology on a part-time basis, on the one hand, while 69% of students described themselves as such that study pharmacology on a full-time basis, on the other, is being indicative that the qualitative particulars of how both categories of students go about pursuing their educational goals, have only a slight effect on these students’ attitudes towards the idea that the course on CAM should be included in their educational curriculum. In its turn, this allows us to hypothesize that the qualitative essence of students’ responses to the questions, contained in the questionnaire, is being of a largely discursive nature. That is, regardless of whether students study pharmacology on full-time or part-time basis, their growing awareness of CAM’s importance is being rather socially than educationally defined.
Summary
The earlier provided analytical review of literature, and the analysis of the collected empirical data, allows us to summarize this study’s findings as follows:
There is an increased tendency among researchers to discuss CAM therapies as being thoroughly consistent with the conventions of Western medicinal paradigm. In its turn, this can be explained by both: the fact that, as time goes on, the conventions of Western medicinal paradigm become increasingly affiliated with the notion of ‘usefulness’, and the fact that the very realities of today’s living naturally cause more and more people to think of their healthiness in terms of a ‘commodity’. The first trend will eventually result in the full legitimization of CAM therapies, as such that despite being often criticized on the account of their implicational ambivalence, do help patients to improve their health-condition. The second trend will result in patients being provided with more and more opportunities to remain in a full control of the process of being subjected to a specific medicinal treatment. Therefore, the idea that pharmacy students should be provided with an opportunity to learn about CAM therapies appears being discursively plausible – by becoming thoroughly familiarized with these therapies, students will able to increase the extent of their professional adequacy.
The fact that, as of today, more and more patients appear to become increasingly comfortable with the idea of being subjected to CAM therapies is best discussed as the one among many extrapolations of an ongoing discursive progress in the field of Medicare, rather than merely the extrapolation of patients’ intellectual arrogance. The validity of this statement is being thoroughly consistent with the present study’s empirical findings, which suggest that the extent of people’s emotional comfortableness with CAM therapies positively correlates with the extent of their intellectual advancement. In its turn, this is being suggestive of the fact that, instead of creating obstacles on the way of CAM therapies legitimization, orthodox physicians/pharmacologists should consider the inclusion of these therapies as an integral of the Western medicinal paradigm. Despite the fact that, as it was illustrated throughout this study’s theoretical part, there are indeed many reasons to doubt CAM’s capacity to serve as the symptom-focused ‘cure’, patients’ exposure to CAM has long proven rather indispensible, within the context of physicians striving to improve the overall extent of patients’ emotional well-being. Given the fact that, as physicians are being well aware of, ensuring patients’ emotional comfortableness often appears to be the foremost prerequisite of their eventual recovery, there can be very few doubts as to the fact that courses on CAM should become an integral part of pharmacological learning.
The analysis of study participants’ responses to the questions, contained in the questionnaire, points out to the fact that; whereas, the majority of students appear being rather knowledgeable of CAM, and also the fact that most of them would indeed welcome the inclusion of CAM-course, as a part of their studies, they nevertheless seem to access the value of CAM therapies from an essentially euro-centric perspective. That is, they tend to regard these therapies as being capable of alleviating the acuteness of a particular symptom, rather than being helpful within the context of patients striving to ensure their long-term ‘healthiness’. This, of course, negatively affects the actual quality of students’ understanding of how CAM therapies may be successfully applied. This problem, can be successfully dealt with by the mean of encouraging students to think of CAM therapies as such that help patients to restore their ‘healthiness’, rather than as such that merely serve a supplementary role, within the context of how patients are being subject to the conventional therapies.
Students’ responses are also being suggestive of the fact that, while answering the questionnaire-based questions, they never ceased being affected by a number of purely societal factors. In their turn, these factors affected the qualitative essence of this study’s empirical findings. For example; whereas, the increased extent of students’ social integration (sandwich course students) appears to have helped these students to remain particularly open-minded about the idea that CAM should indeed be studied by future pharmacologists, these students’ affiliation with other life-pursuits made it more difficult for them to welcome the idea that, along with studying conventional pharmacology, they should also be required to study CAM. This points out to the fact that there is a certain rationale in believing that, contrary to some students’ clearly defined tendency to remain skeptical about the prospect of being required to study CAM; they nevertheless are being generally comfortable with the idea.
Even though that, as it was illustrated by this study’s empirical findings, some pharmacology students exposed themselves being not thoroughly enthusiastic about the prospect of CAM-course’s inclusion into their already intense educational curriculum, the majority of study’s participants expressed their support to the idea. Apparently, students’ responses to the questions, contained in the questionnaire, do reflect their growing awareness of the whole scope of potential benefits, associated with CAM therapies. This, of course, supports the overall legitimacy of this study’s initial thesis.
Conclusion
As it was mentioned in the Introduction, the very realities of a post-industrial living establish objective preconditions for healthcare professionals to grow increasingly open-minded about the idea that CAM therapies should eventually attain a fully legitimate status. As Geigle and Galantino (2009, p. 225) pointed out, “The increasing popularity of CAM reflects changing needs and values in modern society in general, including a rise in the prevalence of chronic disease, public access to worldwide health information, a sense of entitlement to quality of life, interest in spiritualism and a decline of faith that scientific breakthroughs will provide answers for personal treatment of disease”. Therefore, it will only be logical to assume that it is being only the matter of time, before courses on CAM therapies will become fully integrated into the procedural matrix of Western medical/pharmaceutical education. As it was being implied throughout this study’s entirety, such an eventual development is being dialectically predetermined, as the groundbreaking breakthroughs in the field of medicine, which had taken place during the course of recent decades, do substantiate the validity of a theoretical premise, behind CAM therapies.
Even though that, as of today, there is no effective methodology for ensuring the practical insightfulness of CAM therapies’ clinical trials, an ongoing exponential progress in the field of Medicare will result in such a methodology’s eventual emergence. In the light of what has been said earlier, the idea that pharmacy students should be taught about CAM therapies, appears thoroughly plausible. By being provided with an opportunity to learn about CAM therapies, they will not only be able to increase the level of their professional excellence, but they will also be able to serve the needs of a community better. There are many good reasons to believe that the realization of this fact, on the part of students that participated in this study, did affect the qualitative essence of their responses to the questions, contained in the questionnaire. Apparently, while studying pharmacology, on the one hand, and while existing in a socially integrative mode, on the other, it is being rather natural for students to become increasingly aware of CAM’s importance.
Given the qualitative specifics of students’ responses, it will only be logical to suggest that the future studies, concerned with investigating the discursive legitimacy of CAM-courses’ inclusion into the educational curriculum of pharmacology-related studies, should aim at exploring the extent of pharmacology students’ awareness of what constitutes the theoretical premise, behind CAM therapies, and revealing the qualitative aspects of how students envision they should proceed with acquiring relevant knowledge about CAM.
We believe that this conclusion is being thoroughly supported by the review of previous researches, on the investigated subject matter, and by the analysis of the obtained empirical data.
References
Astin, J 1998, ‘Why patients use alternative medicine: Results of a national Study’, JAMA: Journal of the American Medical Association, vol. 279, no.19, pp. 1548-53.
Baarts, C & Pedersen, I 2009, ‘Derivative benefits: Exploring the body through complementary and alternative medicine’, Sociology of Health and Illness, vol. 31, no. 5, pp. 719-733.
Bakx, K 1991, ‘The “eclipse” of folk medicine in Western society’, Society of Health and Illness, vol. 13, no. 5, pp. 17–24.
Bishop, F, Yardley, L & Lewith, G 2006, ‘Why do people use different forms of complementary medicine? Multivariate associations between treatment and illness beliefs and complementary medicine use’, Psychology & Health, vol. 21, no. 5, pp. 683-698.
Colom, F & Vieta, E 2011, ‘The need for publishing the silent evidence from negative trials’; Acta Psychiatrica Scandinavica, vol. 123, no. 2, pp. 91-94.
Colquhoun, D 2007, ‘Head to head: Should NICE evaluate complementary and alternative medicines?’, BMJ, vol. 334, no. 5, pp. 506-507.
Franses, P & Paap, R 2001, Quantitative models in marketing research. Cambridge University Press, Cambridge.
Finkler, K 1994, ‘Sacred healing and biomedicine compared’, Medical Anthropology Quarterly, vol. 8, no. 2, pp. 178-197.
Geigle, P & Galantino, M 2009, ‘Complementary and alternative medicine inclusion in physical therapist education in the United States’, Physiotherapy Research International, vol. 14, no. 4, pp. 224-233.
Kayne, S 2009, ‘Delivering complementary and alternative medicine’, in: S Kayne (ed), Alternative and complementary medicine, Pharmaceutical Press, London, pp. 43-92.
Kayne, S 2009, ‘Introduction to the complementary concept of healthcare’, in: S Kayne (ed), Alternative and complementary medicine, Pharmaceutical Press, London, pp. 3-21.
Kelner, M et al. 2006, ‘How far can complementary and alternative medicine go? The case of chiropractic and homeopathy’, Social Science & Medicine, vol. 63, no. 10, pp. 2617-2627.
Lary, J. et al. (1999) The return of thalidomide: Can birth defects be prevented? Drug Safety, 21(3), 161-169.
Leckridge, B 2004, ‘The future of complementary and alternative medicine-models of integration’, Journal of Alternative & Complementary Medicine, vol. 10, no. 2, pp. 413-416.
Levack, W 2009, ‘Ethics in goal planning for rehabilitation: A utilitarian Perspective’, Clinical Rehabilitation, vol. 23, no. 4, pp. 345-351.
Park, C 2002, ‘Diversity, the individual, and proof of efficacy: Complementary and alternative medicine in medical education’, American Journal of Public Health, vol. 92, no.10, pp. 1568-1572.
Pietroni, P 1987, ‘Holistic medicine: New lessons to be learned’, Practitioner, vol. 231, pp. 1386–1390.
Reast, J, Palihawadana, D & Shabbir, H 2008, ‘The ethical aspects of direct to consumer advertising of prescription drugs in the United Kingdom: Physician versus consumer’, Journal of Advertising Research, vol. 48, no. 3, pp. 450-464.
Rubin, H & Rubin, R 1995, Qualitative interviewing: The art of hearing data. Sage, Thousand Oaks.
Shang, A et al. 2005, ‘Are the clinical effects of homoeopathy placebo effects? Comparative study of placebo-controlled trials of homoeopathy and allopathy’, Lancet, vol. 366, no. 9487, pp. 726-732.