Introduction
The cost of health care has grown tremendously over the past few decades, necessitating the need for the implementation of efficient strategies to cut down healthcare spending. Various scholars have come up with proposals on the best ways to deal with the ballooning cost of healthcare without compromising its quality (He & Mellor, 2013). The current nursing practice involves treating patients as and when they desperately need healthcare. Patients suffering from chronic illnesses receive treatment only when they visit a healthcare facility. Health care providers rarely conduct follow-ups after treating patients. The system is not only harmful to the patient but also practitioners and medical insurance companies. For patients, it leads to the severity of a disease thereby posing a great risk to the patient besides increasing the workload of healthcare providers (Berry, Rock, Houskamp, Brueggeman, & Tucker, 2013). Health insurance firms suffer huge costs resulting from the emergency treatment of the patient. This paper examines the strategies used by modern hospitals to counter the rising cost of health care. To achieve this objective, the paper explores the healthcare system practiced at Gundersen using qualitative and quantitative research methods.
Gundersen Healthcare System
Gundersen refers to a group of hospitals whose headquarters are in La Crosse, Wisconsin (Masterson, Pfaff, Dettmering, & Fleis, 2016). It operates several facilities and services in the nearby counties. The hospitals offer a wide variety of services that are either inpatient or outpatient. As of 2015, the hospitals employed more than 4,500 physicians who worked on a full-time basis across all the branches (Masterson et al., 2016). In addition to physicians, the hospital is an employer of many professionals ranging from nurses to clinical officers. The hospital is credited for high-quality services especially for patients suffering from chronic illnesses. It is important to note that chronic illnesses are highly attributed to the high cost of health care due to numerous emergency cases resulting from poor management (Masterson et al., 2016). The system was launched in 2003 in Gundersen to increase the quality of care for patients with high-risk profiles. The system promotes coordination between healthcare providers to improve healthcare provision and reduce the cost of health care.
Research Methodology
This paper utilized a mixed-method approach (quantitative and qualitative methods) to uncover the strategies that Gundersen Healthcare System used to improve the quality of care for patients with complex health profiles. The qualitative method involved the use of interviews to solicit data from the participants. The quantitative method, on the other hand, involved collecting data using online surveys. The use of the two methods contemporaneously was informed by the view that it would facilitate the collection of sufficient data to test the hypothesis. Also, it would increase the reliability of the data since the information from each tool would be compared with that collected through the other tool.
Sample Population
The study recruited participants from a cross-section of physicians and nurses from the Gundersen Healthcare System. A total of 6 physicians and 4 nurses were recruited for the study. To qualify for inclusion in the study, the respondents had to meet the following inclusion criteria.
- Must have served as a physician or a nurse under the system for at least five years
- Must have basic computer skills and be conversant with the internet
- Had to demonstrate a high understanding of the system’s operations
- Had to be serving patients with a complex health profile
Data Collection Instruments
Interviews
The study conducted one-on-one interviews with the participants to solicit the relevant data to answer the research question. The interviews took place at the participants’ respective places of work. Each participant was given a maximum of 2 hours in which they answered the questions posed by the researcher. The interviews were recorded using video and audio recorders and replayed at the end of the sessions. At this stage, the respondents were at liberty to make the relevant adjustments to the information given to reflect the exact information they intended to pass.
Online Surveys
Online surveys were used alongside the interviews to solicit quantitative data from the participants. The online surveys contained open-ended questions that were designed to collect as much data as possible. The surveys were distributed to the participants via their respective emails. To make sure that the respondents gave reliable data, the researcher prepared a survey guide for the participants. The guide contained information regarding the objective of the study and information about answering the questions. The guides were distributed to the respondents 2 weeks before the commencement of the study. This gave the respondents enough time to prepare for the research to increase the credibility of the responses.
Data Analysis
Both sets of data were compared to assess their reliability and validity. The two aspects were tested by checking the consistency of data given by each participant in each of the tools. Only the consistent data were considered for analysis to ensure the results reflect high levels of credibility. The other step involved sorting out the data whereby similar responses were grouped and assigned unique codes. The codes were used to identify each set of data. The codes would then be input into a computer for analysis.
Results
The study found that Gundersen Healthcare System greatly increased patient outcomes by employing modern healthcare strategies. Among the strategies that the system employ include Continuum of Care, Accountable Care Organizations (ACOs), Medical homes, and Nurse-managed health clinics. The listed strategies were cited by the respondents as being crucial to the improvement in patient outcomes. In addition to the improved patient outcome, the system also reduced healthcare costs by a big margin.
Discussion
Continuum of Care
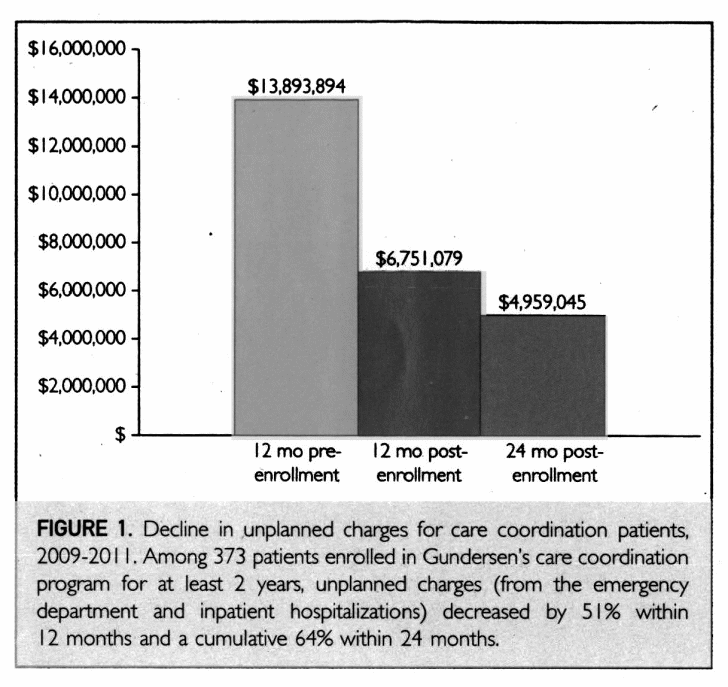
The study revealed that one of the strategies that Gundersen Healthcare System uses is the Continuum of Care. The mentioned concept refers to the continuous monitoring of a patient to mitigate the escalation of his or her illness (Maeda et al., 2014). Under the system, nurses collaborate with physicians to ensure that patients with complex healthcare profiles are continually monitored. Under the continuum of care, nurses not only offer healthcare services to the patient but also offer to follow up services to monitor those suffering from chronic illnesses from their homes (He et al., 2013; Maeda et al., 2014). The role of nurses under the continuum of care changes from that of providing primary healthcare to that of the provision of acute care, ambulatory care, home care, extended care, and wellness programs just to mention a few (He et al., 2013). The result is that the hospital has managed to bring down the number of inpatients since most patients are treated from their homes. The study revealed that the system reduced the number of emergency cases by 51% in 2011 as illustrated by Figure 1 below (Berry et al., 2013). Additionally, the strategy increased the overall patient outcome
The current nursing practice involves treating patients as and when they desperately need healthcare. Patients suffering from chronic illnesses receive treatment only when they visit a healthcare facility seeking medical care (Berry et al., 2013). The system is not only harmful to the patient but also the practitioners and the medical insurance companies. It leads to the severity of a disease posing a great risk to the patient and increasing the workload of healthcare providers. Health insurance firms suffer huge costs resulting from the emergency treatment of the patient (Berry et al., 2013). Therefore, the embracement of the strategy by Gundersen Healthcare System is a major strength since it reduces the overall number of emergency cases, which reduces the overall cost of healthcare in turn.
Accountable Care Organizations (ACOs)
The study also uncovered the use of Accountable care Organizations (ACOs) in Gundersen Healthcare System. The participants credited the strategy for improving the overall patient outcome and reducing the cost of care. ACOs refer to groups made up of providers and suppliers of healthcare services that work together to facilitate the provision of medical care to the Medicare beneficiaries that they serve (Gu et al., 2014). The groups are usually made up of hospitals, nurses, physicians, and other stakeholders responsible for facilitating the provision of healthcare services to the patients. ACOs under Gundersen Healthcare System has greatly changed the face of healthcare by insisting on patient-centered services as opposed to traditional fee-for-service care (Gu et al., 2014). The role of nurses under the system changes from that of providing basic care to managerial roles whereby nurses are empowered to manage a group of healthcare professionals. Nurses are required to embrace research to facilitate evidence-based practices. Under ACOs, nurses are tasked to ensure that the cost of health care goes down to achieve savings owing to the requirement that nurses bear some financial risks for their patients (Gu et al., 2014).
As indicated in the table below, the study observed that Gundersen Healthcare System managed to reduce the overall fees charged to patients by 39% within 1 year. The reduction in the charges was higher in the next period as the hospital achieved a cumulative reduction in healthcare costs by 60% over 2 years (Berry et al., 2013). This illustrates that ACOs, as employed under the system is effective in reducing healthcare cost and other hospitals across the globe need to implement it to achieve similar benefits.
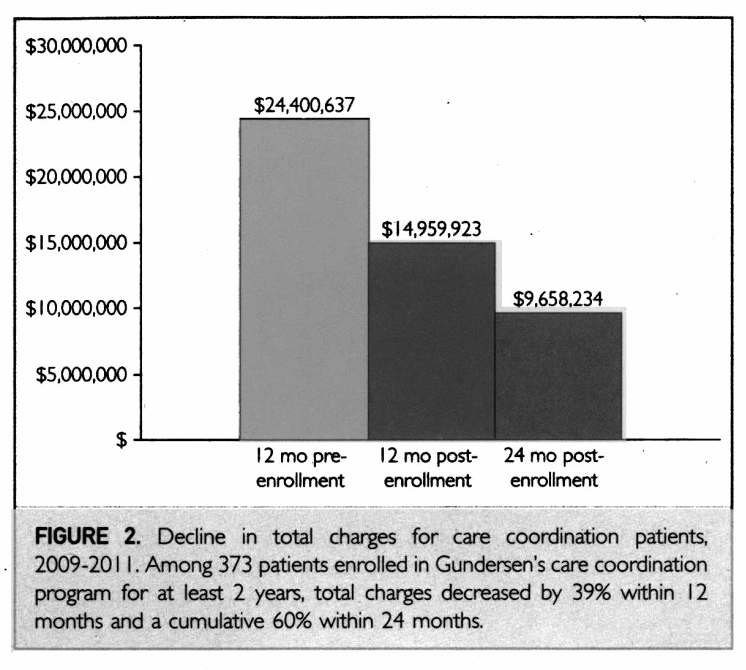
Medical Homes
Another concept that the researcher found applicable in the Gundersen is that of medical homes. The medical home healthcare model involves the creation of a patient-physician long-term relationship to facilitate lasting health (White, Carney, Flynn, Marino, & Fields, 2014). It seeks to replace the episodic care that is currently in place in most healthcare facilities in the US. The adoption of the model in Gundersen follows the view that there might be a shortfall of healthcare providers in the future against the backdrop of the aging population and the increasing number of patients suffering from chronic illnesses (White et al., 2014). Based on the concept of medical homes, nurses have their roles changed from traditional episodic care to managerial roles whereby they are charged with the responsibility of managing healthcare for a group of patients. They also act as the intermediaries between the patients and the physicians.
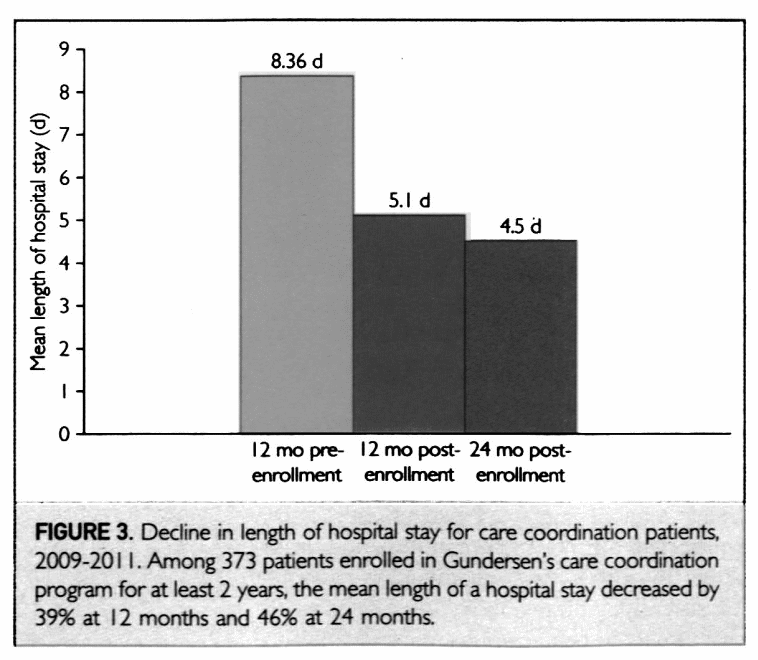
In Gundersen, the nurses act as the intermediaries between the physician and the patient so that they continuously monitor the patient and refer the patient to a physician as and when the patient needs such intervention. The concept ensures that all patients get access to the physicians in the backdrop of the few physicians. As stated earlier in this paper, Gundersen only has 4,500 physicians who must serve the high population of patients in the counties of operation (Berry et al., 2013). Without such a concept, many patients would not have a chance to meet a physician. Additionally, the concept ensures that a patient gets access to a physician as and when his or her situation demands the intervention. The timely intervention of a physician helps reduce the length of stay for patients admitted to hospitals. As indicated in the figure below, the hospitals managed to reduce the length of hospital stay by 36% and 49% for 1 year and 2 years respectively (Berry et al., 2013). Such a reduction in a hospital stay can lead to a significant reduction in healthcare costs.
Nurse-Managed Healthcare Clinics
Lastly, the study found that Gundersen utilized the concept of Nurse-managed health clinics to increase patient outcomes and to reduce the cost of health care. A nurse-managed healthcare center refers to clinics managed by nurses and offers medical care to patients in underserved areas (Burke, Guo, Prochazka, & Misky, 2014). The clinics’ chief aim is to seal the gap in the provision of health care for both uninsured and underinsured persons across the counties. In most cases, nurses work independently. In some clinics, nurses collaborate with physicians to facilitate the provision of quality services to the patients (Burke et al., 2014). The concept of nurse-managed health clinics promotes the independence of nurses in the backdrop of the increasing number of patients. Under the concept, the role of nurses can be altered from that of junior members in the healthcare fraternity to that of certified healthcare providers (Burke et al., 2014). By utilizing the strategy, Gundersen manages to reduce the number of inpatients since nurses closely monitor the patients from the most convenient locations. Additionally, nurses are empowered to give relevant advice to patients with a view of promoting self-care.
Conclusion
In the recent past, the cost of health care has increased tremendously prompting major hospitals to device strategies to contain them. The high cost of health care has been attributed to the lack of proper management of chronic illnesses. Many people suffering from such sicknesses often require regular checkups to mitigate the escalation of the illness. However, the conventional healthcare system does not recognize the importance of continuous treatment for such patients. This situation leads to the intensification of the illnesses. In emergencies, patients consume a lot of resources, a situation that leads to the ballooning of healthcare costs. Besides, it predisposes a patient to the risk of death, which may be prevented if better treatment methods were adopted. This paper has explored the evolving strategies for managing patients with complex health profiles concerning the Gundersen healthcare system. The study adopted a mixed-method approach to collect and analyze data from the participants.
References
Berry, L., Rock, B., Houskamp, B., Brueggeman, J., & Tucker, L. (2013). Care coordination for patients with complex health profiles in inpatient and outpatient settings. Mayo Clinic Proceedings, 88(2), 184-194.
Burke, R., Guo, R., Prochazka, A., & Misky, G. (2014). Identifying keys to success in reducing readmissions using the ideal transitions in care framework. BMC Health Services Research, 14(1), 423.
Gu, Q., Koenig, L., Faerberg, J., Steinberg, C., Vaz, C., & Wheatley, M. (2014). The Medicare hospital readmissions reduction program: Potential unintended consequences for hospitals serving vulnerable populations. Health Services Research, 49(3), 818-837.
He, D., & Mellor, J. (2013). Do changes in hospital outpatient payments affect the setting of care? Health Services Research, 48(5), 1593-1616.
Maeda, J., Henke, R., Marder, W., Karaca, Z., Friedman, B., & Wong, H. (2014). Association between the unemployment rate and inpatient cost per discharge by payer in the United States, 2005–2010. BMC Health Services Research, 14(1), 378.
Masterson, C., Pfaff, B. L., Dettmering, C., & Fleis, J. (2016). Creating a sustainable culture of safety related to hand hygiene in an integrated health system. American Journal of Infection Control, 44(6), 8.
White, B., Carney, P., Flynn, J., Marino, M., & Fields, S. (2014). Reducing hospital readmissions through primary care practice transformation: This study found that a” culture of continuity” using processes that strengthen outpatient-inpatient caregiver communication improves patient care. Journal of Family Practice, 63(2), 67-75.