Describe how cultural practices can promote good physical and mental health, as well as how they can discourage good physical and mental health. Provide an example for each. List a cultural practice that you grew up with or that you believe in strongly that is a health benefit. Please remember to describe it for those of us who might be unfamiliar with the practice!
Some cultural practices may enhance the promotion of health awareness while others may inhibit it. The effects of cultural practices affect the domains of both physical and mental health: “Culture helps to determine how one feels about health and illness” (Skolnik, 2011, p. 18). For instance, the significance of family bonds and the cooperation between the members of the family, which the African American culture can be characterized by, serves as an important tool for improving the quality of the therapy provided to the patients. The lack of trust that the Russian immigrants treat healthcare services with, in its turn, leads to the development of serious health issues, primarily physical ones (Purnell, 2014).
The emphasis on cooperation, which implies active engagement and empathy of not only family members but also friends and the representatives of the community can be viewed as the primary characteristic of the Native American tradition (Hernandez, Nesman, Mowery, Acevedo-Polakovich, & Callehas, 2015). The identified philosophy can be viewed as essential to the faster recovery of the patient as it contributes to both the increase in their awareness regarding their health issues and the redesign of their values. For instance, the patient may be convinced by his community to adopt a healthier lifestyle by reconsidering their diet. Although the Native American practices also imply the use of shaman’s help, which may complicate the treatment process, the significance of family values can be viewed as essential to the success of the therapy in this case.
What are the most important ethical concerns that arise when research is conducted with people in developing countries? In your opinion, do you think that U.S. companies should or should not utilize subjects from other countries? Why or why not?
When researching developing countries, one must make sure that the rights of the research participants should be acknowledged and that the people participating in experiments should not be exposed to health risks. Particularly, the trials mustn’t be “exploiting poor people for the gain of people in developed countries” (Skolnik, 2011, p. 77). Therefore, it is recommended that the outcomes of the trial should be beneficial primarily to the people that participate in the experiment.
I believe that U.S. companies should utilize subjects from other countries in their research as long as the participants of the trials are provided with an opportunity to use the medicine produced as a result of the experiment either for free or at a very low price. Thus, the people living in the target area will be provided with an opportunity to receive the necessary healthcare services. Besides, the participation in the trials should be on a strictly voluntary basis, with the possible threats being clarified to the participants in detail. Another essential restriction concerns the age of the participants – they should be at least 21 to take part in experiments (McRae et al., 2013).
If you wanted to encourage large-scale healthy behavior change in a community, such as quitting cigarette smoking, what information would you need to know in the planning phase of your effort?
Carrying out a massive change in the mindset of a community is challenging primarily due to the lack of understanding of the values and traditions that the community in question thrives on. To be more accurate, the healthcare services aiming at carrying out the change will have to conduct an extensive analysis of the culture of the community to learn about the imagery that can be used in the campaign to get the message across faster. Moreover, the verbal component of the message will be delivered more accurately as soon as the information regarding the specifics of the community culture is retrieved.
Thus, the premises for a better understanding of the current behavioral patterns adopted by the members of the community can be identified. As soon as the researcher realizes what the current behavioral patterns are shaped by, the tools for making the necessary change to the patterns in question can be identified. Therefore, for making a change to a specific community and enhancing the significance of a healthy lifestyle in the target area, one must collect the data related to the traditions and values upheld by the residents of the area. As long as the crucial cultural drivers are identified, it will become a possibility to detail the approach to be adopted.
Which principles could be used to justify a decision about how to allocate care resources in health care?
The issue of healthcare resource allocation can be viewed as rather debatable, as Skolnik (2011) explains. In the countries with high GDP, while the quality of the healthcare services is rather impressive, the waiting time leaves much to be desired. Therefore, the time-related issues can be deemed as one of the factors that should define the allocation strategy. For instance, the areas where patients need to be provided with the treatment immediately, have to be funded firsthand.
In developing countries, where the financial circumstances of most citizens can be described as dire, the lack of opportunities for providing healthcare services to the people that cannot possibly pay for it should be viewed as the factor determining the funds’ allocation. Specifically, it is recommendable that the facilities located in low-income communities should be provided with the necessary financial resources first (Porney et al., 2013).
Based on the speculations above, it will be sensible to assume that the principle of sustainability should be used as the primary tool in distributing the financial resources among healthcare facilities. Reaching out to the communities with low-income families is a crucial step toward a massive increase in people’s quality of life. Thus, the corresponding values can be interpreted as the primary principles for allocating care resources. However, addressing the time management issue, i.e., reconsidering the staff’s schedule, the current hiring techniques, the staff’s competencies, etc., is also a necessity. In light of the problems mentioned above, the concept of sustainable use of resources (i.e., the allocation based on need and urgency) must be promoted as the primary one.
Why are environmental health issues important in global health? Which environmental health issue is most important? Why?
Although the tidal wave of environmentalism seems to have died down over the past few years, the necessity to incorporate the information concerning the current environmental status of specific areas with the health programs and changes to be implemented is still evident. First, the investment schemes drafted to provide the necessary health services to the people living in remote areas depend heavily on the environmental specifics of the areas in question: “Many readers will be familiar with an environmental assessment of proposed investment schemes, and many countries require such assessments be done before any major physical investment” (Skolnik, 2011, p. 129).
Apart from the financing issue, the correlation between the environmental concerns and the emergent health issues needs to be addressed. Seeing that none of the ecosystems on the planet can be viewed as entirely isolated from the rest, the slightest changes in one of the domains will inevitably trigger a range of alterations in the others, creating a global pattern. The inhabitants of the areas, in their turn, will be exposed to risks related to the changes in the environment and the emerging hazards. Thus, the local environmental issues affect the local health concerns to a considerable extent.
According to the reports submitted by WHO (2016b), water pollution poses the greatest threat to global health. Although other concerns can also be deemed as important, the lack of clean water is a problem that needs to be addressed in a manner as efficient and expeditious as possible. Affecting children and adults alike, it causes health complications and often deaths from dehydration.
Describe the links between nutrition and health. What parts of the world have the worst nutritional problems? What do you do as a student to maintain balance and good nutrition?
The connection between nutrition and health is evident. By consuming food, which contains a specific amount of fats, carbohydrates, and proteins, people receive the necessary amount of energy that will sustain them throughout a specific period. Moreover, the nutrients that food consists of sustaining the biological development of an individual. For instance, studies point to the fact that the children that do not receive the necessary amount of nutrients face the risk of developing severe health complications: “poor nutritional status in infancy and young childhood may be linked with several non-communicable diseases, including diabetes and heart disease” (Skolnik, 2011, p. 19).
Overconsumption of food, however, also leads to the development of health issues, such as obesity and the following risk of CVD, diabetes, and other disorders. As far as the lack of food is concerned, developing countries have the greatest problems with nutrition (see Fig. 1). The states that are currently viewed as economic leaders, in their turn, show rather high rates of obesity and the related issues (CVD, diabetes, etc. (see Fig. 2)).
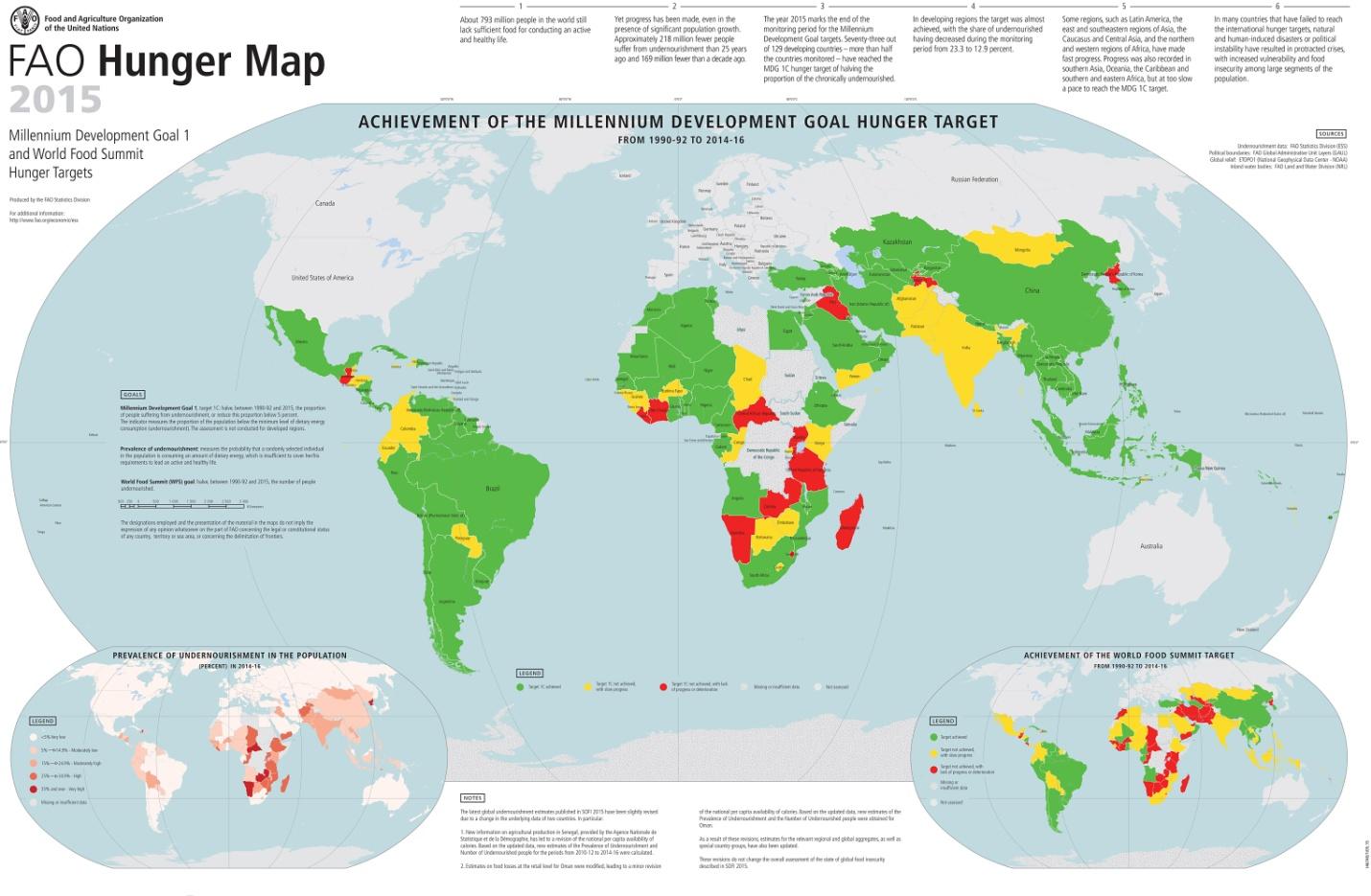
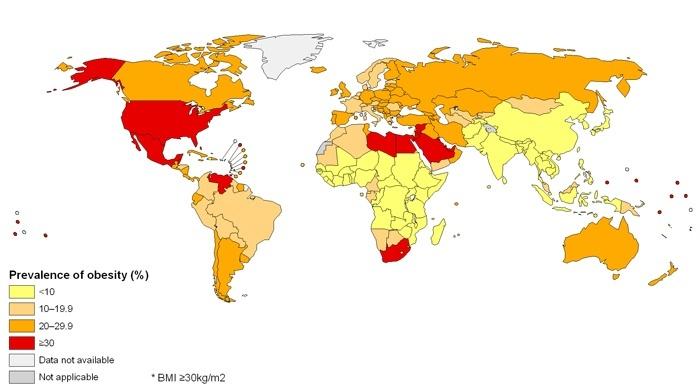
As a student, I prefer to maintain balance when it comes to the nutrition process. For instance, I follow a healthy diet that helps me remain in control of my weight as well as the number of nutrients received daily. Also, I coordinate my diet with the pieces of advice provided by the therapist. Moreover, I focus on what I eat, avoiding soda, sweets, food that contains fats, etc.
In what regions of the world is the indoor pollution problem greatest? Why? What types of things can you do at home to improve your air quality?
Although the issue of indoor pollution (IAP) has been raised by WHO with the help of both traditional and modern media quite a few times, the levels of IAP are still unreasonably high. Typically defined as the “smoke in and around the home” (WHO, 2016d) and usually caused by the use of solid fuels as the means of cooking and heating the house, IAP affects people’s health to a considerable extent. According to the latest report on the subject matter, the subject matter is especially topical for the residents of developing countries (WHO, 2016b). With little to no opportunity for using the resources that could help them improve the air quality, people in the developing regions such as India, Benin, Iraq, Bhutan, etc. have no other choice but to use the fuel that increases IAP levels.

To improve the air quality, one should consider the use of improved ventilation, as well as air cleaners. The latter collects pollutants from indoor air, therefore, creating a healthier environment (EPA, 2016). Also, the transfer to a greener approach toward using fuel should be viewed as a necessity. Last but not least, I do not smoke; as a result, the rates of IAP are reduced significantly.
What are some of the direct and indirect causes of undernutrition?
Undernutrition is one of the scourges of the 21st century that affects not only people’s physical health but also their mental capabilities, including the ability to process information in a fast and logical manner: “Children that do not have access to clean water and sanitation are more likely to suffer from undernutrition due to a vicious cycle of diarrheal disease and malnutrition” (Skolnik, 2011, p. 142). This calls for the identification of the primary causes of undernutrition and the design of the strategies that will help remove the causes in question.
As a rule, poverty is mentioned as the primary cause of malnutrition (Muller & Krawinkel, 2005). Often related to poverty, war as the key factor, and lack of education as the direct consequence thereof are traditionally listed among the leading cause of undernutrition. Insufficient food security is also related to the issue of undernutrition, as it can be viewed as the direct effect of poverty. Besides, an unhealthy environment is often rendered as one of the major causes of undernutrition. In children, the lack of parental care – or, in case of the parents’ absence, the lack of care of the child’s legal guardians needs to be mentioned as the source of undernutrition.
What are some of the key differences in the burden of disease between males and females? Why is particular attention paid to the health of females? This topic of women’s health is very important and goes beyond the concept of healthy mom healthy baby. We deal with many of these issues here in the U.S. including FGM. What are some of your top issues that occur with women?
At present, the focus of the disease burden analysis is on women (). The gender differentials as far as the levels of mortality and morbidity are concerned can be viewed as the key reasons for the emphasis on the effect that the disease burden has on female patients. Besides, by considering only women when addressing the problem of the contemporary disease burden, one is likely to identify the issues that women face when consulting the corresponding nursing and healthcare services.
Indeed, a closer look at the subject matter will show that, due to the past trials that used to focus on male participants only, the current ideas about the application of certain types of medicine to meet the female patients’ needs might be a touch biased. As a result of following the specified practices, one is likely to face a range of problems when tending to the needs of female patients. In other words, there is a necessity to focus on the health issues that women face to provide them with the required treatment and offer the services of the stated quality.
Considering the validity of the phenomenon, one should bring up the fact that differential access to social protection mechanisms is currently practiced in a range of areas. Moreover, the fact that there is a considerable biological difference between the male and female patients should be listed among the primary factors that define the course of the contemporary disease burden studies (Buvinic, Medici, Fernandez, & Torres, 2007).
What are the most important unintentional injuries affecting children? Are there cost-effective ways to reduce the burden of these injuries? What might you do in the future to safeguard your home for child safety?
Unintentional injuries remain one of the leading causes of death among children and adults alike and often cause disability (Skolnik, 2011). In children, unintentional injuries are typically classified into three large groups. The first one includes the specifics of the children’s temper, their age group, and other individual variables that are likely to increase the possibility of receiving an unintentional injury.
Another vast category includes the characteristics of the family. The identified group is admittedly large, as it incorporates the information about the number of siblings, parental engagement, the support that parents receive when tending to the needs of their children (e.g., babysitting services provided by the family members, etc.), and other relevant characteristics of the environment.
Finally, the community factor should be listed among the crucial ones. The support provided by neighbors is also considered an important contribution to the process of reducing the risks of an injury. Engaging friends, neighbors, and family members in the process of taking care of the children can be considered one of the most cost-efficient tools for creating a safer environment for children. I will ask the family and community members to cooperate to create a safe environment for children. The latter should also be given age-appropriate instructions about household safety and prevention of all kinds of injuries. Thus, a responsible attitude can be fostered in children at a relatively young age, thus, preventing injuries in the future.
What are some cost-effective measures that could be implemented to improve the health of women in low-income countries? What, if any, the difference is there between children in low-income families that live in industrialized countries and those that live in countries that are not industrialized?
Gender issue remains on the agenda of the contemporary health services globally. The problem is especially topical for the residents of low-income countries. To improve the quality of the health services provided to the target members of the population, the state authorities use a set of rather impressive leadership skills to coordinate the actions of the staff and allocate the funds available in a manner as efficient as possible.
Moreover, because of poverty, the priorities of the family members, as well as the members of the community, are shifted toward the pursuit of economic benefits rather than preventing the possible health issues and removing the factors that may be viewed as hazards to people’s health. As Skolnik (2011) states, the timelines of the required services also leave much to be desired in low-income countries: “While preparing dinner one evening, the sleeve of Shahnaz’s outfit dipped into the cooking fire.
Before her family could help her, all of Shahnaz’s clothing was engulfed in flames. Shahnaz died the next day from burns” (Skolnik, 2011, p. 301). The lack of family support should also be noted as one of the crucial characteristics of the relationships between the people from the identified socioeconomic background.
Children from poor backgrounds all over the world seem to face a similar issue. Although living in a low-income family implies facing a range of challenges no matter what country the child resides in, the younger members of low-income families in industrialized states have more options for receiving assistance from the state authorities and the corresponding healthcare programs. Nevertheless, financial support is required for the non-industrialized countries so that the quality of the services could reach the required level.
How does the health of young children in low-income countries vary with the income of the family?
Although the economic environment of low-income countries does not create many premises for the provision of the necessary healthcare services, the income of the family defines the number of services provided as well as the quality thereof. As a result, the health status of children from a positive social and economic background is much higher than the one of the children from poor families. In light of the facts provided above, improving the living standards of the people inhabiting low-income areas should be viewed as the first step to take in improving the quality of care. The rearrangement of the local people’s values should be the next step. Thus, the members of low-income areas will be able to focus on health-related issues, managing them in a timely fashion.
Reference List
Buvinic, M., Medici, A., Fernandez, C., & Torres, A. M. (2007). Gender Differentials in health. In Disease control priorities in developing countries (2nd ed.) (pp. 195-210). Oxford: OUP.
Hernandez, M., Nesman, T., Mowery, D., Acevedo-Polakovich, I. D., & Callehas, L. M. (2015). Cultural competence: A literature review and conceptual model for mental health services. Psychiatric Services, 60(9), 1046-1050.
EPA. (2016). Improving indoor air quality. Web.
McRae, A. D., Bennett, C., Brown, J. B., Weijer, C., Boruch, R., Brehaut. J.,… & Taljaard, M. (2013). Researchers’ perceptions of ethical challenges in cluster randomized trials: a qualitative analysis. Trials, 14(1), 1-7.
Muller, O., & Krawinkel, M. (2005). Malnutrition and health in developing countries. CMAJ, 173(3), 279-286.
Porney, M. P.., Forest, P.-G., Sanmartin, C., DeCoster, C., Clavel, N., Warren, E.,… & Noseworthy, T. (2013).
Purnell, L. D. (2014). Guide to culturally competent health care. Philadelphia, PA: F.A. Davis.
Skolnik, R. (2011). Global health 101. (2nd ed.). New York, NY: Jones & Bartlett Publishers.
The state of food insecurity in the world 2015. (2015). Web.
WHO. (2016a). Deaths from indoor smoke. Web.
WHO. (2016b). Environmental health issues. Web.
WHO. (2016c). Global obesity trends. Web.
WHO. (2016d). Household (indoor) air pollution. Web.