The success of the proposed project’s implementation, a mindfulness meditation program, depends on several factors that could be defined as facilitators and barriers. In the site, there is currently no culture to support evidence-based practice, and staffing levels can affect the implementation because of the necessity to find additional time for education and practice. The expected barriers will include the acceptance of the program by the local community or, in other words, the desire of nurses to participate in this intervention and accept change. Resistance to change is one of the common implications not because of the offered idea but because of the nature of the process to quit old routine (Salam & Alghamdi, 2016). The lack of funding and skilled personnel to cover the needs of participants and the researcher could also challenge the progress of the working process. Finally, the impact of a pandemic remains unpredictable for nurses, patients, educators, and researchers due to poor awareness and experience.
To solve these problems and facilitate the intervention implementation, several strategies are recommended. A leader of the intervention has to be motivated and know how to motivate the participants. The development of communication skills and cooperation contributes to the establishment of trustful relationships. The pandemic progress may be traced by available local data resources about the health situation in the region, the already made achievements, and current challenges. Nurses’ resistance to change can be reduced by the promotion of information via flyers and personal communication to give meaningful explanations and clarify all questionable points. Talking about the capitalization upon facilitators, properly developed qualities such as communication, motivation, and trust will be applied in other research projects, relying on the already obtained experience.
Outcomes
To determine the impact of the intervention, it is important to collect the material from past research and apply data collection and analysis tools correctly. Nursing has already been proved as one of the most stressful professions, especially when nurses should work with high mortality patients (Gholizadeh et al., 2017). In this study, the Expanded Nursing Stress Scale (ENSS) will be used for stress assessment, and the Health Survey SF-12 will help to measure the physical and mental health of nurses (Saedpanah et al., 2016; Sarafis et al., 2016). The ENSS includes 57 questions and is based on a five-point Likert scale to identify emotional needs, working problems, and conflicts among nurses (Gray-Toft & Anderson, 1981). The expected Cronbach alpha level is between 0.8 and 0.9 to prove the test internal consistency reliability. In SF-12, there are 12 questions to identify emotional and behavioral changes, the reliability and validity of which can be checked within the frames of the chosen sample and the results of Pearson correlation analysis (Ware et al., 1996). Finally, a self-administrated test will be applied to gather demographic information about the participants and descriptive statistics for analysis (multiple linear regression).
All the tests and a survey will be administrated personally to every nurse in a written (pen/paper) format. One week is the deadline for participants to answer the questions before the intervention, and the same period is given after the program’s implementation. Before the direct contact with nurses, it is necessary to receive permission from an administrator or a nurse leader to use a survey (the permission letter is attached as Appendix A).
In a self-administrated questionnaire (SAQ), there will be several questions to obtain demographic data with the help of which a PICOT question can be answered. First, all the participants share their gender, age, and nursing experience to prove that they meet the inclusion criteria. Then, they mention several duties in a hospital in relation to patients who are at risk of mortality. This information is necessary in terms of discussing the topic of how a mindfulness meditation program influences nurses’ well-being and abilities to work under a pandemic condition. The questionnaires (ENSS, SF-12, and SAQ) are mentioned in Appendix sections (Appendix B, C, D) for further distribution among nurses approved for this evidence-based practice (Gray-Toft & Anderson, 1981; Ware et al., 1996). Nurses have to be informed about their responsibilities and the deadlines for their answers orally, but they are free to withdraw the intervention any time they want, without explaining the reasons. Regarding the nature of the intervention, in this study, no abstracting data from electronic sources and hospital reports are necessary. Nurses prove their responsibilities when they answer questions and share their current experience in a hospital.
References
Gholizadeh, M., Khademohosseini, S. M., Mokhtari Nouri, J., & Ahmaditahoor, M. (2017). The effect of mindfulness intervention on job stress in nurses of intensive care units. Critical Care Nursing Journal, 10(3). Web.
Gray-Toft, P., & Anderson, J. G. (1981). The nursing stress scale: development of an instrument. Journal of Behavioral Assessment, 3(1), 11-23.
Saedpanah, D., Salehi, S., & Moghaddam, L. F. (2016). The effect of emotion regulation training on occupational stress of critical care nurses. Journal of Clinical and Diagnostic Research, 10(12).
Salam, M., & Alghamdi, K. S. (2016). Nurse educators: Introducing a change and evading resistance. Journal of Nursing Education and Practice, 6(11), 80-83.
Sarafis, P., Rousaki, E., Tsounis, A., Malliarou, M., Lahana, L., Bamidis, P., Niakas, D., & Papastavrou, E. (2016). The impact of occupational stress on nurses’ caring behaviors and their health related quality of life. BMC Nursing, 15(1).
Ware Jr, J. E., Kosinski, M., & Keller, S. D. (1996). A 12-item short-form health survey: Construction of scales and preliminary tests of reliability and validity. Medical Care, 34(3), 220-233.
Appendices
Appendix A
Permission Letter for Conducting Survey
To:
Date:
Sir/Madam,
I am a research scholar in (specify a facility, department). I wish to inform that I am conducting surveys for data collection among the nurses of this hospital who become direct participants of the intervention (give the name). The goal of this evidence-based practice is to measure stress among nurses who work with high mortality patients during a pandemic and introduce a mindfulness meditation program to promote well-being among the nursing staff.
Therefore, may I request your kind permission to conduct surveys among the chosen staff to collect the required data in the form of written questionnaires. All information about the participants will stay confidential and be used for academic objectives only.
Thanking you in advance and best regards.
Yours sincerely,
Mention a name.
Appendix B
Expanded Nursing Stress Scale
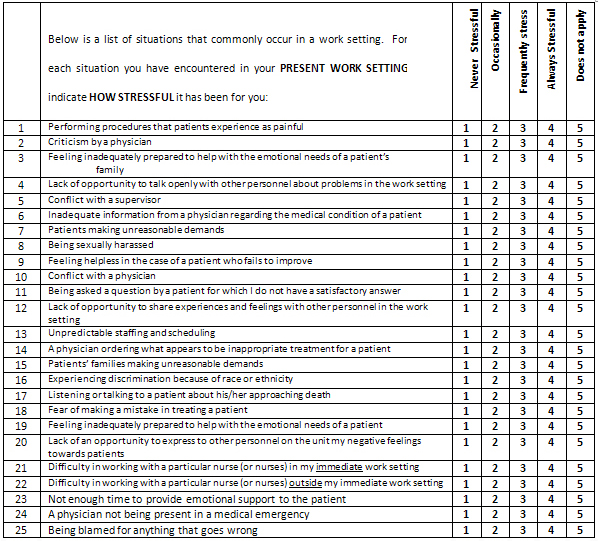
Appendix C
SF-12 Questionnaire
- In general, would you say your health is:
- Excellent (1)
- Very Good (2)
- Good (3)
- Fair (4)
- Poor (5)
- The following two questions are about activities you might do during a typical day. Does YOUR HEALTH NOW LIMIT YOU in these activities? If so, how much?
- MODERATE ACTIVITIES, such as moving a table, pushing a vacuum cleaner, bowling, or playing golf:
- Yes, Limited A Lot (1)
- Yes, Limited A Little (2)
- No, Not Limited At All (3)
- Climbing SEVERAL flights of stairs:
- Yes, Limited A Lot (1)
- Yes, Limited A Little (2)
- No, Not Limited At All (3)
- During the PAST 4 WEEKS have you had any of the following problems with your work or other regular activities AS A RESULT OF YOUR PHYSICAL HEALTH?
- ACCOMPLISHED LESS than you would like:
- Yes (1)
- No (2)
- Were limited in the KIND of work or other activities:
- Yes (1)
- No (2)
- During the PAST 4 WEEKS, were you limited in the kind of work you do or other regular activities AS A RESULT OF ANY EMOTIONAL PROBLEMS (such as feeling depressed or anxious)?
- ACCOMPLISHED LESS than you would like:
- Yes (1)
- No (2)
- Didn’t do work or other activities as CAREFULLY as usual:
- Yes (1)
- No (2)
- During the PAST 4 WEEKS, how much did PAIN interfere with your normal work (including both work outside the home and housework)?
- Not At All (1)
- A Little Bit (2)
- Moderately (3)
- Quite A Bit (4)
- Extremely (5)
- The next three questions are about how you feel and how things have been DURING THE PAST 4 WEEKS. For each question, please give the one answer that comes closest to the way you have been feeling. How much of the time during the PAST 4 WEEKS –
- Have you felt calm and peaceful?
- All of the Time (1)
- Most of the Time (2)
- A Good Bit of the Time (3)
- Some of the Time (4)
- A Little of the Time (5)
- None of the Time (6)
- Did you have a lot of energy?
- All of the Time (1)
- Most of the Time (2)
- A Good Bit of the Time (3)
- Some of the Time (4)
- A Little of the Time (5)
- None of the Time (6)
- Have you felt downhearted and blue?
- All of the Time (1)
- Most of the Time (2)
- A Good Bit of the Time (3)
- Some of the Time (4)
- A Little of the Time (5)
- None of the Time (6)
- During the PAST 4 WEEKS, how much of the time has your PHYSICAL HEALTH OR EMOTIONAL PROBLEMS interfered with your social activities (like visiting with friends, relatives, etc.)?
- All of the Time (1)
- Most of the Time (2)
- A Good Bit of the Time (3)
- Some of the Time (4)
- A Little of the Time (5)
- None of the Time (6)
Appendix D
Self-Administrated Questionnaire
- Gender:
- Age:
- Nursing experience:
- Duties: