Every professional requires his or her knowledge to be up-to-date to stay competent, which cannot be truer in the sphere of nursing (Dyson, Hedgecock, Tomkins, & Cooke, 2009). Rapid changes and the constant arrival of new challenges in practice and theory dictate the need for continuous data refreshment and replenishment (Prideaux, 2007). Additionally, it is in every nurse’s interest to become more and more skilled with each passing day as many lives depend on it (Karseth, 2004). The variety of cases to solve growing with each year urges to learn new techniques to adapt and be ahead of the adversities that lie on the path of the medical worker (Mill, Astle, Ogilvie, & Gastaldo, 2010; Keogh, Fourie, Watson, & Gay, 2010).
According to many researchers in the sphere, and education need assessment (ENA) is a great way to decide where the learning intervention is needed and how to address the problem area (DeSilets, 2007; Dyson et al., 2009). An educational need (EN) arises when professionals sense that their skills or knowledge do not satisfy the requirements imposed by the job or the time in the context of technological advancements. Recognizing and addressing ENs might be a top priority for devising an adequate education program. The knowledge update that would be the result of the implementation of such a program based on ENA findings should bring a major improvement in the quality of care in an intensive care unit (ICU) setting.
Background
The modern nursing practice and theory constantly change in the attempt to deliver the best care for patients. The theoretical background that is developed to shed light on a particular problem is often plentiful. The professionals with full-time occupations may not have the time to cover all of it to complete a well-rounded picture on a certain subject that only vaguely touches his or her everyday practice. The first step to discover the area in which the professional has a gap is to identify ENs through ENA (Turner, Davies, Beattie, Vickerstaff, & Wilkinson, 2006). It has been acknowledged that this system of learning could bring substantial results in the form of wise use of resources eliminating ill predisposition (DeSilets, 2006). According to Forbes, While, and Ullman (2006), there is a considerable body of research that suggests learning activities to be planned by previously determined ENs among the target group. All of this is particularly relevant to King Fahad Specialist Hospital in Qassim where each professional is determined to live up to the highest standards in their sphere.
Data Collection Methods
Sample
The target population for ENA was the ICU nursing staff of King Fahad Specialist Hospital where the author is currently employed. A total of 17 people took part in the ENA activities. The fact that the researcher of the current study is aware of the daily challenges that the unit faces greatly benefited the ENA design and influenced the decision on the target group. In addition, I observed my colleagues and conversed with them on professional topics, which indicated the need for educational interventions.
Those interventions, to my mind, could lie in the sphere of bowel management systems, palliative care, and tube feeding. The reason for that is the professional literature where I have found indications that those were problem areas for some nurses. Additionally, I received confirmation from my colleagues that these topics would help increase their professional competence. My assumptions based on clinical experience and literature on nursing are that my colleagues would prefer to extend their knowledge firstly on bowel management systems, as the cases connected with this sickness are quite frequent in ICU. However, it causes many problems and requires substantial amounts of time to deal with them (García et al., 2012). Secondly, I presume, that tube feeding often becomes an issue because relatives often try to abstain from the practice. At least, if the process is handled by nurses (Mula, Ncama, & Maluwa, 2014). Kim and Choi-Kwon (2011) notice that underfeeding problems are not uncommon in ICU and tube feeding could address them.
Tool Description
A questionnaire was used as a tool for data collection. Other options like an interview or the Delphi technique suggested by DeSilets (2007) were also considered but were dismissed as highly time-consuming. The questionnaire method possesses certain flaws connected to its subjectiveness, as mentioned by Timmins (2015). However, as the easiest and, provided it is adequately structured and approved by professionals, it could yield considerable results. Due to the absence of a standard survey form for IC units, a new one was created. It was designed in collaboration with the ICU nurse managers who assisted in elaborating questions. The corresponding scholarly sources related to survey design cited in the body of this paper were also consulted. The final variant was sent by e-mail to Continuous Medical Education Centre at King Saud University Medical City who gave positive feedback. Given the facts mentioned above, the survey may be viewed as valid.
The elaborated ENA survey consists of three parts: demographic data, choice of most urgent topic, and open-ended questions. There is also an additional, fourth part that covers the type of education tools the target group would prefer (see Appendix A). The first part included only one question that only briefly outlined the professional portrait of a surveyed person. This part should show the presumable relation of education and experience in ICU to the EN. The section did not include other parameters like gender, age, or general experience in nursing because the search for the reasons why a particular individual has a certain piece of knowledge is not the priority of the research. The key question the survey needs to answer is which of the three identified topics is the most relevant to nurses in the context of their education. That will allow us to identify the steps to eliminate the gaps in knowledge.
The most urgent question in the survey is designed to determine the preferences of one subject above the other. This would be used to measure the amount of time to be allocated to each topic in the study course. The open-ended section should provide a better insight into the details of the topic where a person wants to improve his or her knowledge (Rattray & Jones, 2007). The fourth part assisted in understanding the preferences of a group in terms of material presentation and transmission channels and was designed as a multiple-choice questionnaire in two parts. This should also help shape the education plan according to the group’s preferences in learning.
Tool Implementation and Related Difficulties
The tool was created based on a free Google service called ‘google forms’. Therefore, it was distributed online. This decision was made based on the author’s personal observation that most of the potential responders were pretty advanced PC and Internet users. Two colleagues were less proficient, but their involvement was ensured by providing them a chance to fill the form from the other colleague’s laptop evading the access problem.
The option of printing the tool was also considered. It was dismissed due to the manual character of assessing the data, which leaves the possibility of human error during calculation. Above that, there may have been problems with the collection of the printed surveys as they are easily lost or damaged. The online form’s mechanism allows doing the assessment automatically. In addition, it gives the possibility to change the questionnaire later and easily spread it again without the need to reprint and distribute it personally (Hunter, 2012).
17 nurses in the ICU were asked to participate in the survey about their ENs. All 17 people agreed to take part and successfully completed it. They encountered no serious misunderstandings during the process of participation. Survey responses were submitted automatically to the author’s Google Drive upon completion. The name and other personal details were not asked in the questionnaire and were not otherwise collected by Google Forms, so respondents remained anonymous. Therefore, the experiment could be deemed successful. However, some of the partakers forgot to fill the form at first notice and needed to be reminded to do it. There was no difficulty with that, as an e-mail reminder can be composed in a few clicks (Hunter, 2012). If the team was not that well-built and less technologically-minded, people of the previous generation could have fallen out of the survey’s picture.
Data Analysis
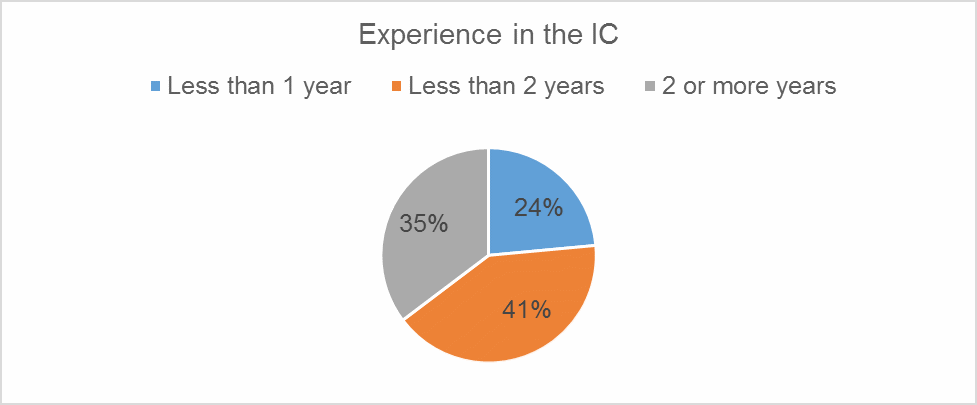
The questionnaire response rate was 100%, which is an excellent result corresponding with the set goals. According to Fincham (2008), even a 60% mark may be considered a success depending on the goals. The demographical section brought the following results: four (23.5%) nurses had ICU work experience under one year, seven nurses had worked in intensive care for less than two years (41%), and six (35.5%) served there for more than two years (see Figure 1).
Tube feeding was chosen as the most urgent topic eight times (47.5%), Bowel management systems – five times (29.5%), and palliative care – four times (23.5%). The results are shown in Table 2.
Table 2. Survey results
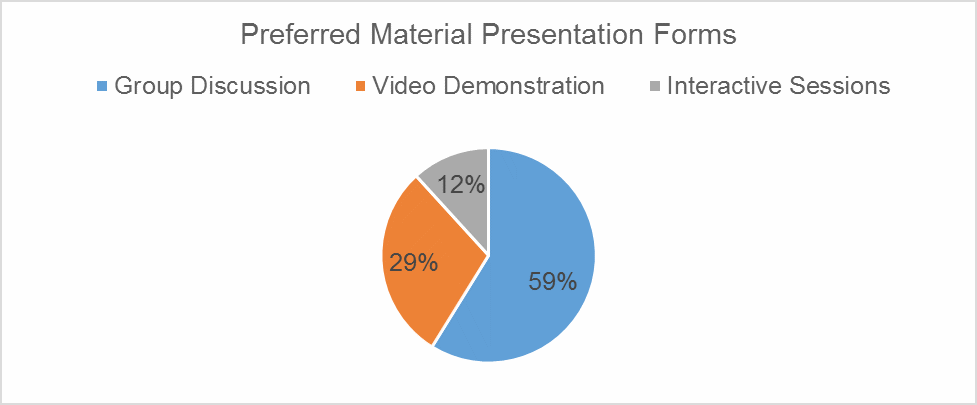
The answers in the first part of the last section divided in the following way: ten nurses (59%) chose group discussions, while five (29%) and two (12%) people voted for video demonstrations and interactive forms of education sessions respectively (see Figure 2). Among respondents, no one voted for lectures, and no one proposed his or her variant.
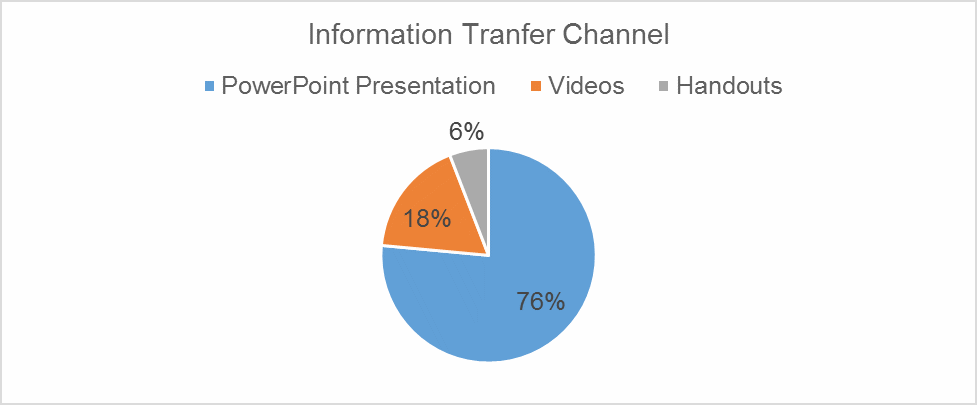
In the second part, where the information transfer channel was chosen the results were imbalanced in favor of PowerPoint presentation with this answer scoring thirteen (76.5%) and Videos – three (17.5%). Also, there was one (6%) vote in favor of handouts (see Figure 3).
Findings
The experience-related part of the survey did not seem to achieve palatable results, as there was no clear pattern of votes spreading following the service term. As to the main question, tube feeding obtained a visible preference among the three. Bowel management systems and palliative care separated by only one point seem to arouse the same amount of interest in nurses. The limitation of this study is in its small representativeness. The present survey only conveys the opinion of a small group of nurses, a single unit. If the research was supposed to survey ten or a hundred different ICUs, the results might not have been the same (Holmes, 2009).
The results of the survey disproved the initial judgment about the leadership of bowel management topic. That situation gives one more evidence to the DeSilets’ (2006) notion that ENA stands above the hypotheses of their creators and even the clinical experience and the fact of acquaintance with participants may be of no help.
In terms of material presentation, it is clear that conventional and now outdated methods like lectures and printed materials are out of favor. Digitized display, on the other hand, is almost universally praised with 76.5% of votes cast for PowerPoint presentation and 17.5% – for video. These findings support the thesis that if utilized correctly, digital and visual-oriented information can positively influence the absorption of information (Nowak, Speakman, & Sayers, 2016). Zero-interest in learning through games may indicate that the unit consists of adult grown professionals who do not easily engage in activities more suited for school-level learning (Boctor, 2013).
Education Programme Plan
Following the results of the study of nurses’ learning preferences, an education program plan was outlined. It will last for four weeks. About the main topic choice, a considerable amount of time will be allocated to tube feeding. Approximately one week with five sessions. Sessions can last for about an hour and a half. It is vital to keep the theoretical knowledge being used for practice (Hatlevik, 2012). Therefore, each PowerPoint lecture and video demonstration of the best tube feeding application should be followed by practical lessons. Hatlevik (2012) also suggests that the bond between theoretical and practical often happens through reflective thinking, which is why a reflection class follows each of the three major topics.
For bowel management systems and palliative care, there will be two weeks organized in the same fashion as tube feeding. However, the sessions will be less frequent. Bowel management systems can sometimes be a hard topic to discuss with patients and their relatives. The education program needs to revise the best strategies to prepare them for it (García et al., 2012). Also, the ethical side of the question needs to be considered as it is viewed as key to good nursing care (McLean, 2012). The practical course should include the proper use of bowel management systems. Palliative care is mostly about providing end-of-life care to patients or providing emotional support after the patient has left ICU (Aslakson et al., 2014). According to Mosenthal (2012), the choice of information-giving strategies is crucial in palliative care. Therefore, the course should also give them some attention. It is also important to revise and critically assess the knowledge that will be gained in the course of these three weeks. In the final week, nurses will indicate the pluses and minuses of the program to adjust it for future use if needed. Table 2 represents the structure and timeline of the proposed education program.
Table 2. Educational program plan
The goal of the above-mentioned plan is to raise the practical education level among the ICU nurses based on their identified self-assessed gaps in knowledge. According to Dalley, Candela, and Benzel-Lindley (2008), it is much more profitable for a nurse to learn narrow topics that give practical knowledge than trying to memorize vast amounts of content in lectures. Such problem-based learning is a good alternative to conventional studying (Martyn, Terwijn, Kek & Huijser, 2014; Vittrup & Davey, 2010) further develop this idea saying that. The present plan made in accordance with experience, scientific knowledge, and evidence may also boost the quality of patient service through the nurses acquiring new knowledge and skills.
Conclusion
The current work represents a research report on the results of ENA tool implementation in ICU nurses employed at King Fahad Specialist Hospital. The tool was devised by the author with the assistance of ICU nurse managers, based on findings of scientific research, and received positive feedback from the Continuous Medical Education Centre. The implementation of the tool gave an insight into the knowledge gaps of the nursing staff and their priorities for eliminating them. Additionally, it provided information about the nurses’ preferred learning styles. ENA disproved the author’s predictions on the learning gaps and preferences, which can once more stress its significance for enhancing educational experiences. Based on the ENA results a draft of the education program plan was created that should help address the learning needs of the King Fahad Specialist Hospital employees bringing the quality of nursing care to a new level and developing their heart, nerve, and brain.
References
Aslakson, R., Cheng, J., Vollenweider, D., Galusca, D., Smith, T. J., & Pronovost, P. J. (2014). Evidence-based palliative care in the intensive care unit: A systematic review of interventions. Journal of Palliative Medicine, 17(2), 219-235.
Boctor, L. (2013). Active-learning strategies: The use of a game to reinforce learning in nursing education. A case study. Nurse Education in Practice, 13(2), 96-100.
Dalley, K., Candela, L., & Benzel-Lindley, J. (2008). Learning to let go: The challenge of de-crowding the curriculum. Nurse Education Today, 28(1), 62-69.
DeSilets, L. D. (2006). Needs assessment. The Journal of Continuing Education in Nursing, 37(4), 148-149.
DeSilets, L. D. (2007). Needs assessments: An array of possibilities. The Journal of continuing education in Nursing, 38(3), 107-112.
Dyson, L., Hedgecock, B., Tomkins, S., & Cooke, G. (2009). Learning needs assessment for registered nurses in two large acute care hospitals in Urban New Zealand. Nurse Education Today, 29(8), 821-828.
Fincham, J. E. (2008). Response rates and responsiveness for surveys, standards, and the journal. American Journal of Pharmaceutical Education, 72(2), 43.
Forbes, A., While, A., & Ullman, R. (2006). Learning needs analysis: The development of a tool to support the on-going professional development of multiple sclerosis specialist nurses. Nurse Education Today, 26(1), 78-86.
García, C. B., Binks, R., De Luca, E., Dierkes, C., Franci, A., Gallart, E.,… & Wyncoll, D. (2012). Prevalence, management and clinical challenges associated with acute faecal incontinence in the ICU and critical care settings: The FIRST™ cross-sectional descriptive survey. Intensive and Critical Care Nursing, 28(4), 242-250.
Hatlevik, I. K. R. (2012). The theory‐practice relationship: Reflective skills and theoretical knowledge as key factors in bridging the gap between theory and practice in initial nursing education. Journal of Advanced Nursing, 68(4), 868-877.
Holmes, S. (2009). Methodological and ethical considerations in designing an Internet study of quality of life: A discussion paper. International Journal of Nursing Studies, 46(3), 394-405.
Hunter, L. (2012). Challenging the reported disadvantages of e-questionnaires and addressing methodological issues of online data collection. Nurse researcher, 20(1), 11-20.
Karseth, B. (2004). Curriculum changes and moral issues in nursing education. Nurse Education Today, 24(8), 638-643.
Keogh, J. J., Fourie, W. J., Watson, S., & Gay, H. (2010). Involving the stakeholders in the curriculum process: A recipe for success? Nurse Education Today, 30(1), 37-43.
Kim, H., & Choi-Kwon, S. (2011). Changes in nutritional status in ICU patients receiving enteral tube feeding: A prospective descriptive study. Intensive and Critical Care Nursing, 27(4), 194-201.
Martyn, J., Terwijn, R., Kek, M. Y., & Huijser, H. (2014). Exploring the relationships between teaching, approaches to learning and critical thinking in a problem-based learning foundation nursing course. Nurse Education Today, 34(5), 829-835.
McLean, C. (2012). The yellow brick road: A values based curriculum model. Nurse Education in Practice, 12(3), 159-163.
Mill, J., Astle, B. J., Ogilvie, L., & Gastaldo, D. (2010). Linking global citizenship, undergraduate nursing education, and professional nursing: Curricular innovation in the 21st century. Advances in Nursing Science, 33(3), E1-E11.
Mosenthal, A. C., Weissman, D. E., Curtis, J. R., Hays, R. M., Lustbader, D. R., Mulkerin, C.,… & Brasel, K. J. (2012). Integrating palliative care in the surgical and trauma intensive care unit: A report from the Improving Palliative Care in the Intensive Care Unit (IPAL-ICU) Project Advisory Board and the Center to Advance Palliative Care. Critical Care Medicine, 40(4), 1199-1206.
Mula, C., Ncama, B. P., & Maluwa, A. (2014). Nurses’ competency and challenges in enteral feeding in the Intensive Care Unit (ICU) and High Dependency Units (HDU) of a referral hospital, Malawi. Malawi Medical Journal, 26(3), 55-59.
Nowak, M. K., Speakman, E., & Sayers, P. (2016). Evaluating PowerPoint presentations: A retrospective study examining educational barriers and strategies. Nursing Education Perspectives, 37(1), 28-31.
Prideaux, D. (2007). Curriculum development in medical education: From acronyms to dynamism. Teaching and Teacher Education, 23(3), 294-302.
Rattray, J., & Jones, M. C. (2007). Essential elements of questionnaire design and development. Journal of Clinical Nursing, 16(2), 234-243.
Timmins, F. (2015). Surveys and questionnaires in nursing research. Nursing Standard, 29(42), 42-50.
Turner, C., Davies, E., Beattie, H., Vickerstaff, J., & Wilkinson, G. (2006). Developing an innovative undergraduate curriculum–responding to the 2002 National Review of Nursing Education in Australia. Collegian, 13(2), 7-14.
Vittrup, A. C., & Davey, A. (2010). Problem based learning–‘bringing everything together’–A strategy for graduate nurse programmes. Nurse Education in Practice, 10(2), 88-95.